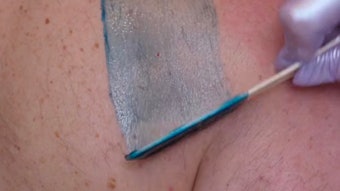
Removing body hair is an important component of daily beauty maintenance for many men and women. However, when your clients have cancer, removing body hair can be more challenging.
Many methods use heat or friction that can cause trauma and provide an entry point for infection, especially for someone undergoing or recovering from cancer. Also, these procedures can be painful, which is elevated with compromised skin. If a spa professional is not educated to work with people that are living with cancer, a simple misjudgement can become unsightly and can cause harm. When dealing with a client with cancer, a lot more thought needs to be put into these hair removal services. This article discusses safety precautions to take with hair removal before surgery, during chemotherapy, during biological therapy and during hormone therapy, as well as additional health considerations.
Hair Removal Before Surgery
When a person is having a surgical procedure in an area of the body that is covered with hair, patients are urged to leave the area of their surgery to the medical team who can complete the task effectively with sterilized clippers.
Waxing. If waxing is preferred, the client should check with the medical team prior to surgery regarding their policies about hair removal and how long prior to surgery this must be done. Any burns or skin removal can create a sore, hence an infection risk. If waxing is a first-time option for the client, they need to take into consideration possible pain and irritation. Any adverse reactions can cause possible cancellation of the surgery.
Tweezing. Tweezing is relatively safe if done correctly without causing any broken skin. Tweezers need to be well sanitized.
Home care. Shaving can cause tiny cuts and abrasions. Where skin is damaged, bacteria can grow and multiply, which can then infect the nearby surgical site. A blade that has not been sterilized also creates a risk by exposing the skin near the surgery site to harmful bacteria. Shaving can also cause folliculitis, an infection in the hair follicle usually caused by the bacteria Staphylococcus (staph) or a fungus. Depilatories can also irritate the skin, so using this cream would not be a good idea prior to surgery if it has never been used before.
During Chemotherapy
Not all chemotherapy drugs cause hair loss; some cause hair thinning or partial hair loss. From a psychological standpoint, hair loss is one of the most feared side effects to treatment, so be aware that hair loss is not a welcome side effect for many. Patients undergoing chemotherapy may have a weakened immune system, which implies they are not ideal candidates for hair removal treatments.
After completing chemotherapy, some women can experience unwanted facial hair brought on by “medical menopause.” This hair can occur approximately one month after the last chemotherapy treatment. Sometimes it resolves on it’s own, but other times the individual may choose to get the hair removed professionally or they do it themselves.
Waxing. Waxing can be extremely painful for someone who is not feeling well during chemotherapy. It may hurt the client to have the hair pulled from the root, and the wax also adheres to their skin, taking skin cells with it as it’s removed. While that is a benefit for people with no health challenges, the client with sensitive, fragile skin affected by chemotherapy drugs may get more irritation and inflammation. This can be exacerbated if the client has a reaction to the chemicals in the wax. If the wax used is too hot, there’s also a risk of burning the skin. If the skin is not held taut when pulling the wax strips off, bruising may occur. Waxing would be high risk for the neutropenic and/or thrombocytopenic client. Also, remember another added skin side effect for this client is dry skin. If the skin is not properly hydrated, it could be more easily irritated, and the risk for tearing the skin is higher.
The melanocytes can also be affected by certain toxic chemotherapy agents, and they can either produce hyperpigmentation, or they can trigger hypopigmentation. Any aggressive wax formulations can ignite the melanocyte activity through cellular trauma; however, the melanocytes are already being affected by chemotherapy agent(s).
Tweezing. Tweezing uses no chemicals that touch the skin, so it’s relatively safe. Removing hair from the root lasts about the same amount of time as waxing. Removing each hair individually using tweezers can be time consuming, and it may be the only option if the skin is experiencing side effects like itching, burning, peeling or stinging. When tweezing, ensure the skin is held taut or you may accidently grab the skin, causing broken skin.
Home care. Shaving brings about the same risks mentioned above. The chemicals in a depilatory cream may irritate the skin causing burning, redness, inflammation, blisters, peeling or a rash, especially if the cream is left on too long. Additionally, the smell of these products can be quite offensive to a person undergoing chemotherapy.
During Biological Therapy
A group of biological therapy drugs such as: Cetuximab (Erbitux), Erlotinib (Tarceva), Gefitinib (Iressa) and Panitumumab (Vectibix) can cause hair loss on scalp, yet increased hair on face and eyelashes. Vandetanib (Caprelsa) can cause hair loss over the entire scalp and reduced hair on legs or arms; can increase the growth and curling of the eyelashes and eyebrows, and increase facial hair growth. These changes don’t usually happen right away, but they may be noticed as treatment continues. This group of drugs may not cause as many adverse reactions to hair removal; however, it must be noted that they can be administered in conjunction with chemotherapy.
Waxing. Waxing is not recommended, as it can irritate sensitive skin and may be a cause for infection.
Tweezing. Tweezing is relatively safe if tweezers have no sharp edges.
Home care. Shaving could also present a risk for infection; however, an electric razor would be a better option to remove any new or increased hair growth. Depilatories may cause a reaction to the skin.
During Hormone Therapy
Aside from the loss of elasticity, skin thinning and dryness, vellus hair on the face becomes a visible problem for women on hormone therapy drugs. Unwanted facial hair is common in menopausal women. An increase in facial/body hair is called hypertrichosis. This group of drugs may not cause as many adverse reactions to hair removal; however, it must be noted that they can be administered in conjunction with chemotherapy.
Waxing. Waxing may cause burning and tearing of the skin. Hot wax may be a better option than strip wax; however, it must be well determined by the spa professional whether the skin can handle any waxing.
Tweezing. Tweezing is relatively safe if tweezers have no sharp edges.
Shaving. Shaving could also present a risk for infection; however, an electric razor would be a better option to remove any new or increased hair growth.
Depilatories. Depilatories may cause discomfort and may irritate the skin.
During Radiation Therapy
Radiation therapy will generally cause hair loss to the body part that is being treated; therefore, the area affected is localized. For example, if the client’s arm was treated with radiation, they may lose hair on their arm, but the hair on their head would not be affected by radiation therapy.
Hair loss may be temporary or permanent, depending on the total amount of radiation received and other treatments such as chemotherapy. When hair loss is temporary, it will likely regrow within three to six months after treatment is complete. The regrowth of hair is often thinner or of a different texture.
Over time, a person who is undergoing external beam radiation therapy may experience fibrosis in the area of radiation. Fibrosis is the formation of excess fibrous connective tissue in an organ or tissue in a reparative or reactive process. This can be a reactive, benign or pathological state. In response to injury, this is called scarring.
In the case of fibrosis, hair is unable to grow through the hardened skin. This can lead to a cessation of hair production and the death of hair follicles.
Waxing. Waxing on areas of skin that has received radiation therapy may be thinner or a different texture. Be aware of any possible neuropathic pain, which could be accompanied by loss of sensation. If hair growth is in an area of irradiated skin, it is not advised to wax over this area. It would be like waxing over a sunburned area, yet over time the skin may be more fibrotic. The heat from the wax can “burn” over an area of previously burnt skin.
Tweezing. Tweezing can be performed if hair is present.
Home care. Shaving can be done using an electric razor in this area of localized skin if hair is present. Depilatories can be used if skin can handle the chemicals and if hair is present.
Health Considerations
Immunosuppression. If the client’s immune system is not functioning as well as it should, their body does not have the same level of protection against infection or against rogue cells that start to show cancerous changes. In addition, some of these immunosuppressive drugs can also predispose the individual to skin cancer through other mechanisms specific to that individual drug. Therefore, the client is at a much greater risk for developing skin cancer and a range of skin infections. Often these infections develop in unusual ways that can be easily missed unless the client is seen by a spa therapist with experience treating those immunosuppressed. Hair removal techniques that minimize trauma to the epidermis, such as trimming or use of depilatory creams, should be discussed with patients who are immunosuppressed.

Diabetes. It has been suggested that approximately 60% of people with diabetes will develop cancer in their lifetime, so also knowing about diabetes can be beneficial.
Steroids. The client who is taking steroid medication as part of cancer treatment may experience thin or fragile skin which can bruise and tear, which may lead to infection. Any hair removal services that could cause tearing of the skin and create a risk for infection should not be done while using such medication, and not until three months after completing the treatment or when the skin has recovered somewhat to its new normal.
Folliculitis. Folliculitis is the name given to a group of skin conditions where there are inflamed hair follicles. The result is a tender red spot, often with a surface pustule. Folliculitis may be superficial or deep. It can affect anywhere there are hairs, including chest, back, buttocks, arms and legs.1 Eosinophilic folliculitis is a specific type of folliculitis that may arise in some immune suppressed individuals such as those with human immunodeficiency virus (HIV) or those who have cancer. Bacterial folliculitis is commonly due to Staphylococcus aureus. If the infection involves the deep part of the follicle, it results in a painful boil. Drug-caused folliculitis may be caused by the intake of corticosteroids, protein kinase inhibitors (epidermal growth factor receptor inhibitors) and targeted therapy drugs, such as Vemurafenib (Zelboraf) and Dabrafenib (Tafinlar) for metastatic melanoma.
Moles. Raised moles and abnormal looking moles should not be shaved, nor should hair removal services be applied to these moles. Any abrasions on the skin, broken skin and bruises should not have hair removal services applied to those areas. Hair clipping can be performed by cutting the hair growth using a small razor comb and surgical scissors specifically for this purpose. Spa professionals who specialize in hair removal have a close-up view of the skin and can help save a client’s life. Training is available for estheticians that allows them to spot (not diagnose) suspicious moles, to encourage the client to see their physician.
After Treatment
Hair removal services can be resumed after cancer treatment when the skin integrity has improved to its new normal. For each individual, this could be anything from four weeks to six months or more. Remember, some individuals have to be monitored for life, and their skin integrity needs to be assessed on a regular basis due to changes to medications and/or side effects.
REFERENCE
- M Durdu and M Ilkit, First step in the differential diagnosis of folliculitis, Cytology Crit Rev Microbiol, Feb 39(1) 9-25 (2013)