Based on an extensive review of scientific literature and the recommendations of recognized melanoma experts, the American Academy of Dermatology (Academy) has released updated evidence-based guidelines for the treatment of melanoma, the deadliest form of skin cancer.
Published online in the Journal of the American Academy of Dermatology, the Academy’s new guidelines of care for primary cutaneous melanoma focus on biopsy techniques, pathology, surgical treatment, (including sentinel the use of lymph node biopsy) and long-term follow-up care.
“Melanoma is a serious public health issue, as the number of cases has been increasing at an alarming rate—especially among younger people,” said dermatologist Ronald L. Moy, MD, FAAD, president of the Academy. “There are many factors that must be considered when diagnosing and treating melanoma, and these new guidelines offer physicians clinically sound recommendations on how to treat melanoma patients and potentially increase their chance of survival from this deadly disease.”
Melanoma is characterized by the uncontrolled growth of pigment-producing cells. If a mole is new, different or changing, it should be evaluated by a dermatologist as soon as possible. Melanoma incidence rates have been increasing for at least 30 years. Since 1992, incidence rates among Caucasians have increased by 2.8% per year in both men and women.
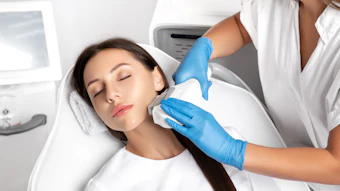
The first step for a definitive diagnosis of cancer is a biopsy of the lesion. If melanoma is diagnosed, the primary treatment is surgical removal of the lesion and surrounding tissues.
It is estimated that there will be 123,590 new cases of melanoma diagnosed in the U.S. in 2011 — 53,360 noninvasive (in situ) and 70,230 invasive. Dermatologists agree that the treatment of noninvasive melanoma (in situ) and invasive melanoma have some differences but also some key similarities. The guidelines explain that with a diagnosis of invasive melanoma, a detailed patient history is imperative and a thorough examination of the skin and lymph nodes should be performed to determine the extent of the spread of the disease. However, for patients with melanomas of any thickness, the guidelines do not recommend baseline blood tests and imaging studies because clinical research does not support their use unless suspicious signs and symptoms are present.
“Melanoma treatments should always be tailored to meet individual patients’ needs,” said Moy. “To ensure the most successful treatment, early detection of melanoma is essential. Studies show that the five-year survival rate for people whose melanoma is detected and treated before it spreads to the lymph nodes is 98%.”
Melanoma patients have a significantly increased risk of developing additional melanomas. The guidelines recommend at the minimum an annual follow-up with a dermatologist, but range from every three to 12 months based on the individual’s history and risk factors. All melanoma patients should perform monthly skin self-examinations. To download a body mole map and learn how to perform a self-exam, visit www.aad.org/checkspot.