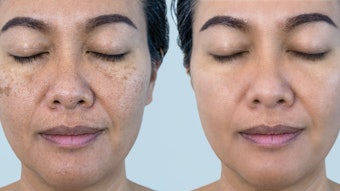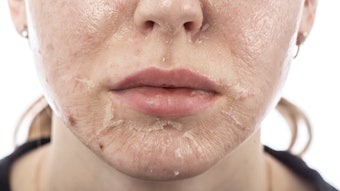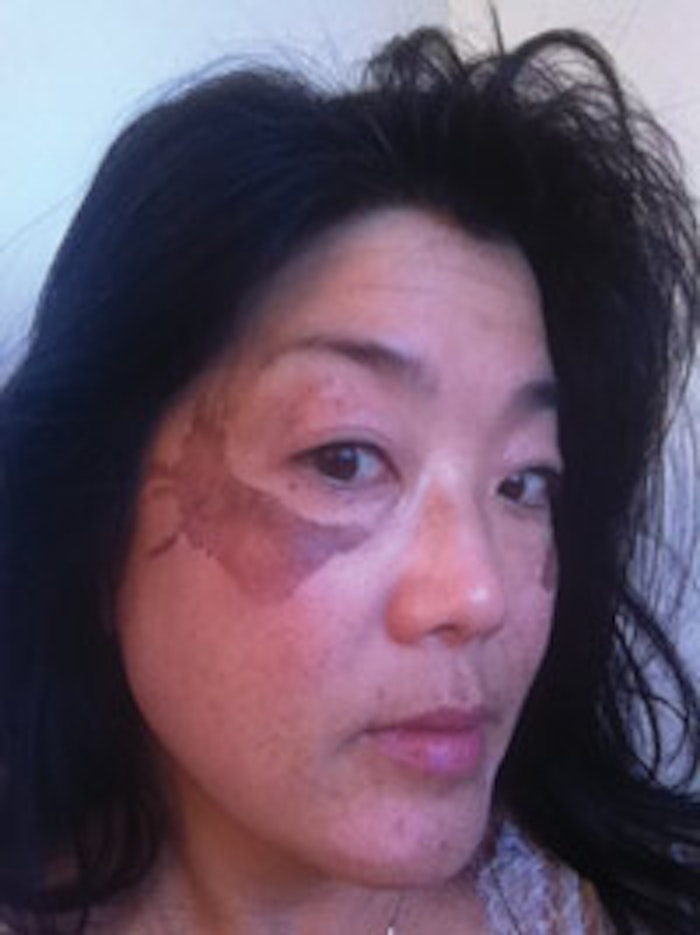
Global skin of color is the ultimate future snapshot of your skin care clientele. Skin care professionals who ignore the phenomenon of the multitude of skin races are out of touch with the reality concerning the trends that will dictate their esthetic careers in the near future, and will miss the opportunity to learn how to work with this ever-increasing population successfully. Skin care professionals must prepare for this prospect, and learn to recognize what is appropriate and inappropriate concerning skin treatments, ingredients and products for skin of color.
There are significant differences between global skin types. Just look at the rainbow of skin colors that make up the millions of skin types and where they originate. Cosmetically speaking, black skin has a wide range of color variations from a creamy light coffee color to deep ebony black. Asian skin exhibits colors that range from a light yellow hue to a dark golden tan. Native American skin colors vary with respect to different tribes, and have coloring that ranges from light to dark red-brown. Even white skin is misinterpreted visually and put into inaccurate categories. Caucasian skin ranges greatly from milky alabaster white to dark olive tones.
Darker global skin types are much more reactive to topical agents such as alpha hydroxy acids (AHAs), beta hydroxy acids (BHAs), trichloroacetic acid (TCA) and many different ingredients, and are more sensitive to these constituents than Caucasian skin. Unfortunately, many skin care professionals misunderstand the darker global skin combinations and treat skin of color as if it were Caucasian, being overzealous in their procedures and recommending improper skin care products, triggering an inflammatory response leading to unwanted problems. This can result in devastating side effects, such as hypopigmentation and hyperpigmentation. These very avoidable mistakes not only affect the client cosmetically and emotionally, but destroy the trust between client and professional.
Understanding color distinction
Melanocytes, melanin and pigmentation formulate the key color distinction of skin. The content of melanin within keratinocytes determines skin color, with deeply pigmented skin having the highest content of epidermal melanin. Melanin is a complex molecule responsible for the pigment in the skin, hair and eyes. This molecule works to protect by reducing the penetration of UV rays into the skin and subsequently into the nuclei of cells where DNA resides.
It is well-established that there are no racial differences in the number of melanocytes; however, the actual number of melanocytes does differ from one individual to another, and from one anatomical region of the body to another, with the head, neck and forearms having the highest number.
Racial and ethnic differences in skin color are due to the number, size and aggregation of melanosomes within the melanocyte and keratinocytes. Racial or ethnic differences in the size and aggregation of melanosomes within keratinocytes have been clearly established. In Caucasian global skin types, melanosomes are smaller in size than those in black skin and contain less melanin.
It has also been determined that melanosomes are larger, more oval and denser in dark-skinned individuals compared to lighter-skinned individuals. Similarly, not all white and Asian skin has small melanosomes, nor are the melanosomes always aggregated. Total melanin content is greater in people with darker skin compared to those with lighter skin.
The amount of melanin is the very basis of skin-typing classification, an important factor in cataloging skin history for UV radiation reaction. The increase of epidermal melanin content of darker-skinned individuals provides greater intrinsic photo protection. Simply put, higher melanin concentration translates into better photo protection from UV radiation and delays the clinical appearance of photoaging brought on by photodamage, especially in lighter skin types that are more prone to UV burn.
Melanosome groupings are also affected by sun exposure. Asian skin exposed to sunlight has a predominance of nonaggregated melanosomes, whereas unexposed skin has predominately consolidated melanosomes. The effects of UV and visible light on human skin include sunburn, suntan, phototoxic and photoallergic reactions, as well as post-inflammatory hyperpigmentation (PIH).
Post-inflammatory hyperpigmentation (PIH)
One of the most common pigmentation disorders of clients with darker skin is PIH, which is one type of pigmentation morbidity. PIH can be considered the default pathophysiologic response to cutaneous injury of darker global skin of colors. This response is the belief predicated on the labile response of melanocytes to irritation or inflammation. The common link to any pigmentation disorder is inflammation. Darker skin differs from Caucasian skin in its reactivity and clinical presentation. Although ongoing research continues to unveil aggravating factors, significant prudence in understanding this problem still remains to be practiced in the area of ethnic skin disorders to properly manage them.
The basis of pigmentation morbidity can occur as the result of cumulative exposure to UV light, making it a major culprit in melasma, solar lentigines and ephelides. Many medications, cosmetics and inflammatory skin diseases, in addition to adverse reactions to chemical peels, ingredients, pesticides, chemicals, detergents, heat, laser resurfacing, laser assisted hair removal and skin injuries can also be a source of pigmentation disorders.
PIH is caused by one of two mechanisms that result in either epidermal melanosis or dermal melanosis. These constituents of inflammation alter the activity of both immune cells and melanocytes. Specifically, these inflammatory components stimulate epidermal melanocytes, causing them to increase the synthesis of melanin and subsequently to increase the transfer of pigment to surrounding keratinocytes. This increased stimulation and transfer of melanin granules results in epidermal hypermelanosis.
Dermal melanosis occurs when inflammation disrupts the basal cell layer, causing melanin pigment to be released and subsequently trapped by macrophages in the papillary dermis, also known as pigmentary incontinence.
Accept the challenge
PIH is a universal response of the skin and can occur in lighter global skin categories, but is more common in the darker global skin types. This condition can occur at any age and takes place in both females and males. Inflammation is the trip wire to hyperpigmentation, and the skin you treat can have many levels of damage that require assessment to determine how you manage pigmentation disorders according to the information brought to light during the client’s skin history consultation.
Are you prepared to accept the challenges of working with skin of color? Beautiful skin, sex appeal, sophistication and good looks have always been a desire of all cultures. Always assess individual ethnic variability when developing a personal home care program and clinical treatment plan.
Christine Heathman is a licensed master esthetician, massage therapist and burn specialist with more than two decades of clinical practice and research at institutions such as Stanford University in Palo Alto, California, and the University of Utah in Salt Lake City. Honored in 2003 as an industry legend by the American Association for Esthetics, she believes the future of skin care is now.