Melanoma is the deadliest form of skin cancer, accounting for approximately 75% of skin cancer deaths,1 and approximately 9,940 U.S. residents are expected to die from this disease in 2015.2 Melanoma is highly treatable when detected early, but survival rates decline for patients whose melanoma has spread to the lymph nodes and other organs.
Within the last five years, targeted therapy and immunotherapy have emerged as viable treatment options for patients with advanced melanoma. Although these therapies have promising implications, early detection still gives patients the best chance of survival.
Skin cancer experts
Information provided by board-certified dermatologist Rhoda M. Alani, MD, FAAD, Herbert Mescon Professor and chair, department of dermatology, Boston University School of Medicine, and dermatologist-in-chief, Boston Medical Center; and Debjani Sahni, MD, assistant professor of dermatology and director, cutaneous oncology program, Boston University School of Medicine.
Targeted therapy
In recent years, researchers have developed drugs that target BRAF mutations, a type of genetic defect that occurs in more than half of melanoma cases. According to Alani, these drugs have proven to be very effective in “turning off” cancer genes by blocking their reproduction and survival pathways, thus stopping further growth and shrinking tumors.
Although BRAF inhibitors are initially effective, Sahni says, melanomas inevitably develop resistance to these drugs by finding ways to get around the blocked pathway. To combat this resistance, scientists developed MEK inhibitors, another type of targeted therapy drug that blocks this pathway at a different step.
Today, BRAF inhibitors and MEK inhibitors are used in combination to provide more effective, longer-lasting treatment for advanced melanoma. Moreover, because the side effects of these drugs counteract each other, patients treated with both may experience fewer adverse reactions than those treated with either drug alone.
Targeted therapy allows doctors to provide patients with more personalized care based on their specific tumors, Alani says. Researchers are now investigating targeted therapies for melanomas that are not triggered by BRAF mutations, as well as melanoma that occurs on places other than the skin, such as melanoma of the eye (also known as ocular melanoma or uveal melanoma). In the future, Sahni says, doctors may use a combination of three or four targeted therapy drugs to provide even more effective treatment.
Immunotherapy
In addition to recognizing and attacking foreign agents such as infections and cancers, the immune system is also designed to keep itself in check and refrain from attacking the body’s own cells. This natural regulation can be hijacked by cancer to evade a patient’s immune defenses. In recent years, however, researchers have increased their understanding of the immune system, Alani says, allowing them to create immunotherapy treatments to fight melanoma.
According to Sahni, scientists have developed therapies that can block the immune system’s checks on itself, allowing the body’s natural defenses to attack tumors more effectively. Although immunotherapy is only effective in a small proportion of advanced melanoma patients, it often produces long-lasting remission in these patients.
As in targeted therapy, doctors may soon combine multiple immunotherapy drugs to provide more effective treatment. Sahni says early studies into such treatment have yielded impressive results. Although combining immunotherapy drugs may increase the potential for adverse effects on the endocrine and digestive systems, it is possible to manage these adverse effects with appropriate treatment in most cases.
Future prospects
Targeted therapy has been shown to extend life in many patients with advanced melanoma, but the effect is short-lived, as patients typically experience a recurrence of the disease. Although immunotherapy works for fewer individuals, it provides a more long-term response when it does work. Additionally, Sahni says, the use of BRAF inhibitors may create a favorable environment for immunotherapy, so the two drugs could potentially work together to kill melanoma cells.
The future of melanoma therapy may lie in combining both types of treatment, which Alani says would allow doctors to develop a more effective, personalized approach for every patient. She notes that clinical trials in this area have been encouraging.
Future research also may allow doctors to determine which melanoma patients have a higher risk of developing metastatic disease, Alani says. If these patients are identified early, doctors may be able to provide them with therapy to stop the spread of cancer and prevent recurrence.
Early detection
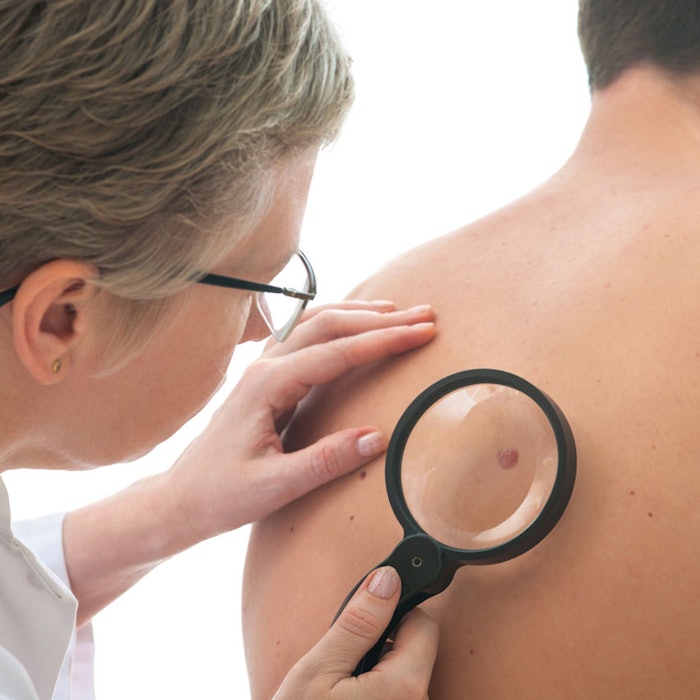
Early detection remains the best way to fight melanoma. Patients whose melanoma is treated before it spreads to the lymph nodes or other organs have a five-year survival rate of 98%; this drops to 63% when the disease spreads to the lymph nodes and other nearby organs, and 16% when it spreads to distant organs.2
The American Academy of Dermatology encourages everyone to perform regular skin self exams. If you notice any spots on your skin that are different from the others, or anything that’s changing, itching or bleeding, make an appointment with a board-certified dermatologist. In addition to investigating suspicious spots, a dermatologist can evaluate your melanoma risk and determine how often you should receive a skin exam in the dermatologist’s office.
Expert advice
“Four years ago, we had nothing to improve advanced melanoma patients’ survival, and now we have several new therapies available, with several others in the pipeline,” Sahni says.
“Although these developments are promising for patients, we don’t have all the answers yet. There’s a lot more research that needs to be done.”
“This is a really exciting time for melanoma therapy. We’re doing all we can to make a dent in this disease,” Alani says. “However, early detection is still vital. The sooner that melanoma is found and treated, the better the patient’s chance of survival will be.”
For more information, contact the Academy at 888-462-DERM (3376) or www.aad.org. Follow the Academy on Facebook (American Academy of Dermatology), Twitter (@AADskin) or YouTube (Academy of Dermatology).
REFERENCES
1 American Cancer Society. Cancer Facts & Figures 2014. Atlanta: American Cancer Society 2014
2 American Cancer Society. Cancer Facts & Figures 2015. Atlanta: American Cancer Society; 2015.