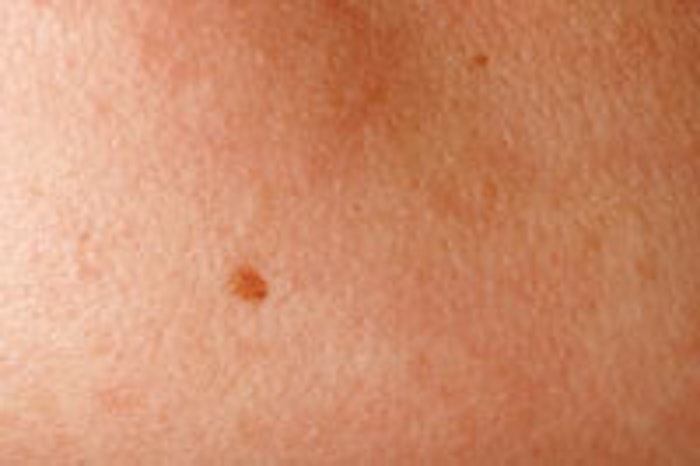
Melanoma is a cancer that appears to start mostly in the skin. The skin has two main layers: the epidermis and the dermis. Deep in the epidermis are cells called melanocytes. Melanocytes make melanin, which gives color to the skin. When skin is exposed to the sun, the melanocytes make more melanin and cause the skin to tan or darken. Sometimes melanocytes cluster together and form moles, called nevi. Moles are common and are usually not cancerous.
There are three types of skin cancer: basal cell carcinoma starts in the basal cells; squamous cell carcinoma starts in the squamous cells; and melanoma starts in the melanocytes.
Melanoma is less common than basal and squamous cell carcinomas. It can start in other places in the body where melanocytes are found, such as the eyes, the mouth or under the fingernails, although these types of melanoma are rare.
A melanoma diagnosis can bring about short- and long-term psychological distress. Skin care professionals who can provide an atmosphere of relaxation and understanding, and have the knowledge of how to handle a client who has undergone treatment for melanoma, can make a hugely positive difference.
Another task that needs to be taken on by skin care professionals is raising the awareness of melanoma in order to save many lives. Public awareness of the danger of sun burns also needs to increase. Skin professionals must encourage people to look for the early stages of skin cancer and to seek medical help. If caught in the early stages, melanoma can be totally cured; however, if it is left unnoticed for too long, it becomes one of the most lethal forms of cancer. It will kill.
Melanoma treatment methods
People with melanoma may opt to treat it through surgery, chemotherapy, radiation therapy, biological therapy or they may undergo a combination of treatments. At any stage of the disease, people with melanoma may have treatment to control pain and other symptoms of the cancer, to relieve the side effects of therapy, and to ease emotional and practical problems. This kind of treatment is called symptom management, supportive care or palliative care.
Surgery. Surgery is the usual treatment for melanoma—the surgeon removes the tumor and some normal tissue around it. This procedure reduces the chance that cancer cells will be left in the area. The width and depth of the surrounding skin that needs to be removed depends on the thickness of the melanoma and how deeply it has invaded the skin. If a large area of tissue is removed, the surgeon may do a skin graft. For this procedure, the doctor uses skin from another part of the body to replace the skin that was removed. Lymph nodes near the tumor may be removed as well because cancer can spread through the lymphatic system. If the pathologist finds cancer cells in the lymph nodes, it may mean that the disease has also spread to other parts of the body. Two procedures are used to remove the lymph nodes.
Sentinel lymph node biopsy. A sentinel lymph node biopsy is done after the biopsy of the melanoma but before the wider excision of the tumor. If a sentinel node contains cancer cells, the surgeon removes the rest of the lymph nodes in the area. However, if a sentinel node does not contain cancer cells, no additional lymph nodes are removed.
Dissection. A lymph node dissection is when all the lymph nodes in the area of the melanoma are removed.
Skin side effects of surgery. Scarring can be a problem for some clients. Generally, scars fade with time, and how noticeable the scar is depends on where the melanoma was, how well the person heals and whether the person develops raised scars, known as keloids. Skin grafts can reduce the scarring caused by the removal of a large growth; however, scars will still be noticeable. Scar tissue is usually weaker, less elastic, more prone to re-injury and can be much more sensitive to pain than normal, healthy tissue. Specialized massage techniques for tissue adhesion can be performed.
Surgery to remove lymph nodes from the underarm or groin area may damage the lymphatic system and slow the flow of lymphatic fluid in the arm or leg. Lymphatic fluid may build up in a limb and cause swelling, or lymphedema. Adjustments need to be made when giving skin care treatments to redirect away from areas of removed lymph nodes and to reduce pressure.
Chemotherapy. Chemotherapy, the use of drugs to kill cancer cells, is sometimes used to treat melanoma. People with melanoma may receive chemotherapy via mouth or injection. Either way, the drugs enter the bloodstream and travel throughout the body.
Through the use of isolated limb perfusion on an arm or leg, chemotherapy drugs are put directly into the bloodstream of that limb. The flow of blood to and from the limb is stopped for a short period of time, allowing most of the drug to reach the tumor directly. Most of the chemotherapy remains in that limb.
Skin side effects of chemotherapy. The side effects of chemotherapy depend mainly on the specific drugs and the dose. In general, anticancer drugs affect cells that divide rapidly, especially the cells of the blood, such as red blood cells, white blood cells and platelets. When white blood cells are very low, a client is more prone to infections, and if the platelets are low, a client is more prone to bruising or bleeding more easily.
Skin care professionals who are not aware of these lab counts and the side effects of chemotherapy should not be working with cancer patients while they are undergoing chemotherapy, because these two side effects can cause some serious issues.
Radiation therapy. Radiation therapy uses high-energy rays to kill cancer cells through the use of a large radiation therapy machine that directs radiation at the body. The patient usually has treatment at a hospital or clinic five days a week for several weeks. Radiation therapy may be used to help control melanoma that has spread to the brain, bones and other parts of the body. It may shrink the tumor and relieve symptoms.
Skin side effects of radiation. The side effects of radiation therapy depend on the amount administered and the area being treated. Side effects that may occur in the treated area include erythema, and possible sensitivity and dryness. Skin care professionals need to avoid working on skin that has undergone radiation during treatment and only start once the skin has healed completely.
Biological therapy. Biological therapy is a form of treatment that uses the body’s immune system, either directly or indirectly, to fight cancer or to reduce side effects caused by some cancer treatments. Biological therapy for melanoma uses substances called cytokines. The body normally produces cytokines in small amounts in response to infections and other diseases. In some cases, biological therapy administered after surgery can help prevent melanoma from recurring. For patients with metastatic melanoma or a high risk of recurrence, interferon alpha and interleukin-2 may be recommended after surgery.
Skin side effects of biological therapy. The side effects of biological therapy vary with the type of treatment. These treatments may cause flulike symptoms, such as chills, fever, muscle aches, weakness, loss of appetite, nausea, vomiting and diarrhea. Patients may also experience a skin rash. These problems can be severe, but they go away after treatment stops. Skin care professionals need to get permission from the client’s physician to work with clients while they are undergoing treatment.
Handling melanoma in the skin care facility
As a skin care professional, what can you do to provide safe treatments to this client aggregate? First of all, make sure to complete comprehensive medical intake forms. If your client is immune-suppressed due to an organ transplant, or has undergone a bone or stem cell transplant and chemotherapy, there is a good chance that she is at risk for squamous cell carcinoma. There is evidence that immunosuppression can lead to squamous cell skin cancer. This increased risk applies to clients with acquired immunodeficiency syndrome (AIDS) as well as transplant recipients on chronic immunosuppressive medications. The risk of developing primary melanoma in the setting of immunosuppression is less well-established, but there is some evidence that clients who have a history of melanoma are more likely to develop disease recurrence in the setting of immunosuppression.
Screening and referring
Skin care clients with numerous benign nevi—small, regularly shaped and uniformly pigmented moles—are at increased risk of melanoma. The same applies to clients who have few dysplastic nevi—large, irregularly shaped and heterogeneously pigmented moles. Patients in either group may have a five-times increased risk of developing melanoma compared with those with few benign nevi or without dysplastic nevi. However, it is critical to recognize that these preexisting moles represent a risk factor for melanoma, rather than precursor lesions, in most cases. The vast majority of dysplastic nevi do not give rise to melanoma.
If a mole on the body has been dismissed by a physician as “nothing” and is changing, this is serious. A changing mole is a dangerous one and always needs evaluation. By performing self-skin examinations on a regular basis, clients and skin care professionals have the power to detect changing moles and bring them to the attention of a doctor. When melanoma is caught in the earliest stages, it’s almost 100% treatable.
Education
As with sun exposure, recent studies indicate a relationship between the use of tanning beds and malignant melanoma, as well as nonmelanoma skin cancers, such as squamous and basal cell carcinomas. Thus, the consequences of regular tanning bed use may include disfigurement from the removal of skin cancers and early death if the cancer is a malignant melanoma, as well as substantial costs for screening, treating and monitoring skin cancer patients. Young adults should be discouraged from using indoor tanning equipment and restricted access to tanning beds by minors should be strongly considered.
Prevention
With the incidence of melanoma still rising, it is clear that primary prevention efforts have not yet taken hold. The only approach firmly rooted in evidence is to minimize sun exposure. The use of sun-protective clothing appears to be the next best strategy. There is conflicting data regarding the protective effect of suncreens for melanoma, although there is no controversy regarding their ability to prevent basal and squamous cell carcinoma. Protection against UVA has been a long-standing feature of widely available suncreens, whereas UVB protection has more recently been engineered into all mainstream products. It is possible that the increased widespread use of these broad-spectrum sunscreens will provide more meaningful protective effects throughout the coming decades.
A new option is becoming available for early melanoma detection in the ability to test for the mutation of the cyclin-dependent kinase inhibitor 2A (CDKN2A) gene. This mutation has been linked to a very high risk of melanoma and was recently the focus of a study reported in the May 2011 issue of Genetics in Medicine. All people with a family history of melanoma showed a reduction in anxiety and depression after getting tested. Patients in this study had a strong family history of melanoma, with at least three relatives affected by the disease. These same patients who tested positive for the high-risk gene became more likely to use sunscreen and to undergo regular skin examinations by a physician for early melanoma detection.
Psychosocial
Personality is associated with health status and the impact of cancer among melanoma survivors. In the field of medical psychology, the Type D personality has a distinct negative impact on health status in melanoma survivors and is an important factor to screen for in clinical practice. Individuals with this personality type have the tendency to experience increased negative emotions throughout time and situations, and tend not to share these emotions with others, because of fear of rejection or disapproval. Giving special attention to these clients is important, because they are more likely to experience a strong impact of cancer that cannot be explained by sociodemographical or clinical characteristics.
Once clients have finished treatment for melanoma, they may still be overwhelmed by emotions. This is the time for all melanoma patients to seek out emotional and social support. They need to find people who they can turn to for strength. Support can be found by caring skin care professionals who will put themselves out there to provide a place of solace and who are certified in esthetics for cancer patients and survivors. They will be assured that their chosen therapist can provide them with a safe and beneficial treatment.
Rewarding work
Any skin care professional who recognizes any form of skin cancer in clients will be emotionally and psychologically rewarded for making the difference in—and possibly saving—the life of a client.
GENERAL REFERENCES
F Mols, C Holterhues, T Nijsten and LV van de Poll-Franse, Personality is associated with health status and impact of cancer among melanoma survivors, Eur J Cancer 46 3 573–580 (Feb 2010)
International Agency for Research on Cancer Working Group, The association of use of sunbeds with cutaneous malignant melanoma and other skin cancers: A systematic review, Int J Cancer 120 11 2526 (Jun 2007)
A Tyndall, JM Van Laar, Intense immunosuppression and stem-cell transplantation for patients with severe rheumatic autoimmune disease: a review, Cancer Control 10 1 57–65 (Jan/Feb 2003)
A Frankenthaler, RJ Sullivan, W Wang, S Renzi, V Seery, MY Lee and MB Atkins, Impact of concomitant immunosuppression on the presentation and prognosis of patients with melanoma, Melanoma Research 20 6 496–500 (Dec 2010)
Morag Currin has more than 16 years of spa industry experience, including training and management, and has pioneered an oncology esthetics certification for estheticians. Students learn to incorporate massage techniques for people undergoing cancer therapies, to screen for cancerous skin lesions and to bring cancer survivors’ skin back into balance. Currin developed TecNiche Therapies, a skin care line for health-challenged skin, and is the author of two textbooks on oncology esthetics, including Oncology Esthetics: A Practitioner’s Guide (Allured Business Media, 2009).