The scope of this article is to provide useful tips for rosacea reduction. It is not an expansive discussion of the types and subtypes of rosacea, or the suspected causes of rosacea. The bottom line is: The fundamental cause of rosacea is not known. It is still vigorously being researched by the pharmaceutical industry, academia and other independent researchers.
One of the biggest challenges for our industry is to properly identify rosacea, and then take steps to reduce it. All too often we hear from individuals whose practitioners have told them their chronic skin redness is rosacea, and many have been provided anti-inflammatories, antibiotics and/or other topicals or oral medications to treat it. Other mechanisms could be involved, an overview of which is given next.
Skin Surface Bacteria
The highest volume of referrals we receive, when standard approaches to treat rosacea fail, relates to surface skin bacteria. Having resident bacteria on the skin surface is normal. Colonies typically are composed of several common species, the majority of which are a type called Gram-positive bacteria. For most individuals, the quantity and types of bacteria do not cause issues.
When bacteria start to proliferate on the skin surface, however, and higher levels of sebum or oil are present, the stage is set for skin challenges to form. Bacteria generally consume and metabolize oil on the surface of skin, breaking it down into a variety of compounds including free fatty acids (FFA). FFAs can have an irritant property, so they can cause chronic skin inflammation over time.
The fix for this is fairly simple but needs to be well-understood to be effective. The objective is to reduce the concentration of Gram-positive bacteria on the skin. The best way to do this is to use a bacteriostatic agent, which stops the bacteria from reproducing. Farnesol is one example, but others are commercially available in topical products. Bacteriostatic agents are different from bactericidal compounds, which kill the bacteria. Benzoyl peroxide, for example, is a bactericidal. The distinction between these is important, as bactericidal compounds can significantly irritate the skin.
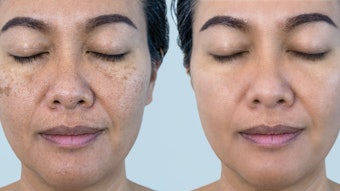
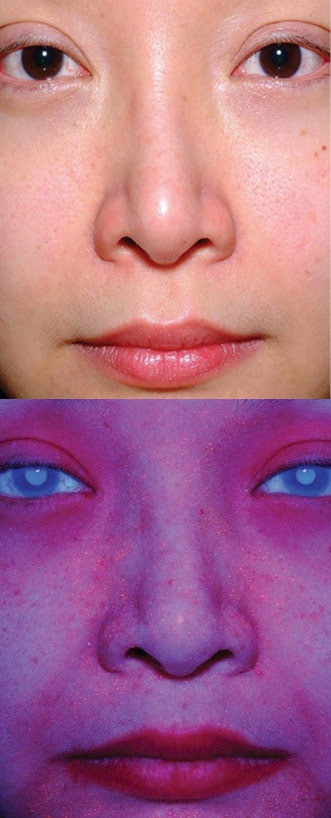
 Bacteriostatic compounds should be used daily. They will slowly reduce the population of skin bacteria and, in many cases, skin redness over time (7-10 days). The best way to apply a bacteriostatic agent is to use a cleanser containing it. Since bacteriostatic compounds are typically oily in nature, the skin will attract them nicely from the cleanser formula. Bacteriostatic Treatment shows the effectiveness of this approach before and after a two-week treatment.
Bacteriostatic compounds should be used daily. They will slowly reduce the population of skin bacteria and, in many cases, skin redness over time (7-10 days). The best way to apply a bacteriostatic agent is to use a cleanser containing it. Since bacteriostatic compounds are typically oily in nature, the skin will attract them nicely from the cleanser formula. Bacteriostatic Treatment shows the effectiveness of this approach before and after a two-week treatment.One challenge to using this method, however, is that color reflectance UV imaging is typically required to see the change in bacteria, as shown in UV Imaging. Therefore, as a suggestion, if a client comes in presenting with chronic skin redness and you do not have this imaging equipment, suggest a bacteriostatic cleanser since it is relatively inexpensive. Then let them assess whether it makes a difference. We’ve seen more than 100 cases per year resolved in this manner.
 Barrier Function Impairment
Barrier Function ImpairmentModerate to significant skin barrier impairment also commonly cause chronic skin redness. The skin’s barrier essentially is a combination of skin lipids and corneocytes in the stratum corneum. Its function is to form a semi-permeable membrane to keep toxins and bacteria out of the body, and to allow for the exchange of water, nutrients and oxygen through it. A functioning skin barrier is especially important considering today’s products, which incorporate active ingredients to impart various effects at the skin’s surface.
The functioning of the skin’s barrier is usually determined by measuring a parameter known as trans-epidermal water loss (TEWL). To measure this, a device known as atewameter is placed on the skin surface to capture the small amounts of water vapor emitted from it. Depending on the concentrations emitted, one can determine if there is no skin barrier impairment, moderate impairment or significant impairment. But besides using a biometric technique like this to measure TEWL, the next best thing you can do is ask questions about skin dryness and hormonal changes.
First, ask the client or patient if they have chronically dry skin. If they say yes, provide a deeply hydrating product that uses active ingredients with known barrier repair properties. A moisturizer alone is not enough since the barrier function will remain impaired. In this case, you will hear comments like, “It doesn’t matter what I use, my skin is always dry.” Be aware that remarks like this are common in cases of classic barrier function impairment.
The second thing to be aware of is, when a patient or client ages, particularly women, their sebum or oil levels drop due to hormonal changes in the body. When these levels change, the skin becomes more rigid and less supple. Less oil in the skin generally leads to more rigid and less supple skin, and this is often reported as dryness. We often see individuals with clinically well-hydrated skin complain about dryness when, in fact, the sebum levels are low and their skin is rigid. This is often confused with the property of “dryness.”
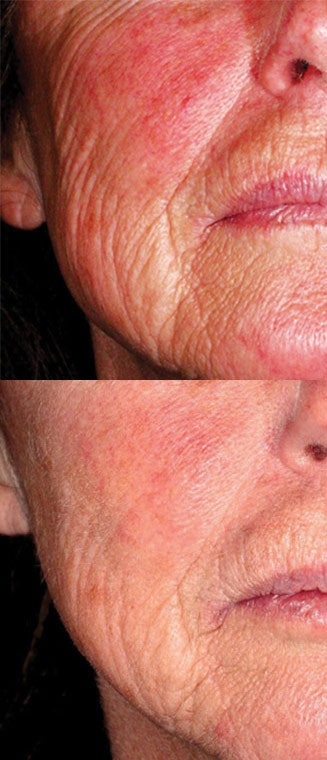
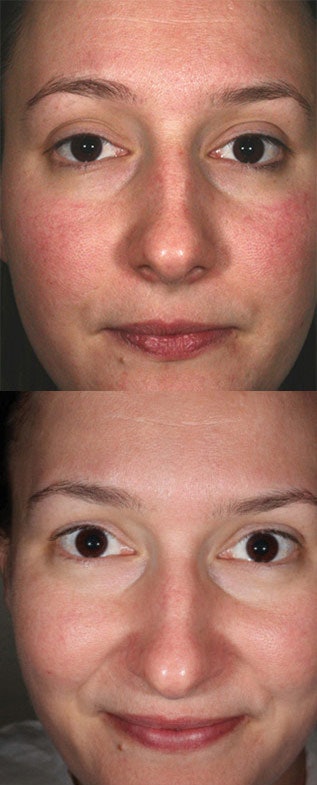 In this case, you can be sure your clients have well-hydrated skin by using lotions and creams that have both barrier function improvement ingredients and sebum-replacement ingredients in them. As an example, caprylic/capric triglyceride is one commonly used sebum replacement ingredient that can provide relief, and it is available in synthetic or natural forms. Barrier Treatment shows skin redness before and after barrier function impairment and normalization, respectively.
In this case, you can be sure your clients have well-hydrated skin by using lotions and creams that have both barrier function improvement ingredients and sebum-replacement ingredients in them. As an example, caprylic/capric triglyceride is one commonly used sebum replacement ingredient that can provide relief, and it is available in synthetic or natural forms. Barrier Treatment shows skin redness before and after barrier function impairment and normalization, respectively.Skin Overtreatment
Over-treating the skin follows the general category of barrier impairment but is more general in nature. In the esthetics industry, there are always new techniques or ways to treat or alter the function of skin, for which some clients may become overly enthusiastic. Here is a short list of what to watch for when treating skin, as these could give rise to acute or chronic skin redness.
Microdermabrasion. When used too often or in combination with silica particles as an exfoliant, microdermabrasion can dramatically compromise skin. The exfoliating particles can raise the pH of skin to higher than nine, which gives rise to short- and medium-term redness due to barrier impairment.
Mechanical devices. Any device that comes into contact with the skin surface for scraping, vacuuming or other purposes must carefully be assessed for frequency of use and any accompanying ingredients that contact the skin.
Dermaplaning. Dermaplaning is a sensitive process that’s relative to the skill and technique of the operator. A non-experienced or too heavy hand can lead to significant barrier impairment, leaving the skin surface in a varied and often compromised condition.
Use of Topicals. The over-use of any ingredient that produces redness is a problem. Benzoyl peroxide, hydroquinone, acids and peels in general should be used carefully, as they act by intentionally interrupting the barrier function. They should be followed by formulas that contain barrier repair ingredients.
Retinoids. It is well-known that retinoids, when used chronically or at too high a dose, can lead to chronic redness—do not recommend them on a regular basis. As an aside, if retinoids, especially prescription types, are used for several or many years without taking a break from them, they can actually atrophy dermal tissue. Instead, using retinoids in an “on and off” frequency will improve chronic redness over time.
Demodex Mites
One additional point to consider: be aware of Demodex mites. We’re learning more and more about these invisible mites, which can leave bacteria behind that may simulate a rosacea response.
Get a History
The final point to make is, since rosacea and/or chronic redness can be difficult to manage, start with three or four questions to help you understand the patient’s basic history. 1) Does your redness/rosacea flare up when you drink wine or alcohol? or 2) or when you perform physical activity? 3) Are you under stress? and 4) Are you taking any medications that are known to cause redness in skin?
Understanding their history, along with the points discussed above, will help you to manage skin redness and provide a level of comfort to your patients and clients.