
That permanent redness that your client is always complaining about is not always rosacea, but can you tell the difference? Here is what you can do to help your client deal with vascular alterations within the skin.
What Are They?
Lesion is the common term for any alteration of the skin that deviates from a normal appearance. The primary and secondary lesions curriculum in school actually are an important concept for skin care professionals to understand when determining what they are looking at. Vascular alterations relate to the structure and function of the cardiovascular system, and it is important to have a general idea of the client’s diagnosed health issues to be able to identify what you see. Also, based on the severity of the vascular lesions, be able to refer them on to a dermatologist.
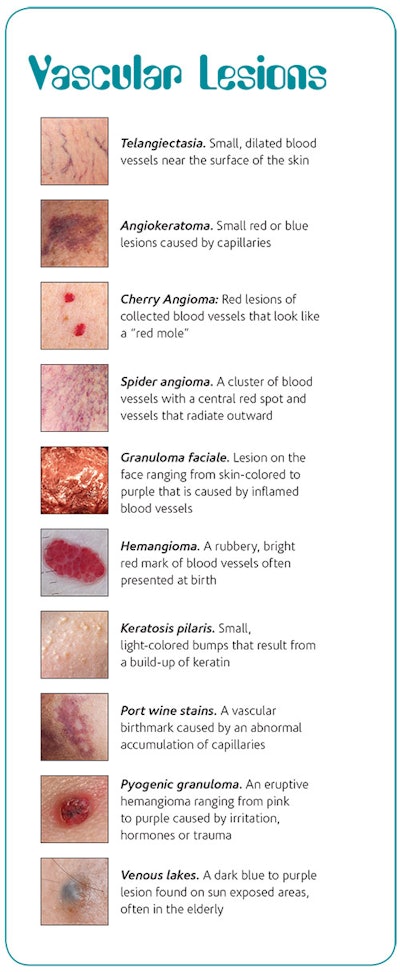
Vascular lesions include the common telangiectasia, angiokeratoma, cherry and spider angioma, granuloma faciale, hemangioma, keratosis pilaris, port wine stains, pyogenic granuloma and venous lakes (see Vascular Lesions). Inflammatory disorders can be involved as well, but is important to note that inflammation or edema do not necessarily mean there is an inflammatory process happening. The common term cuprose is not a medical term, even though it is found in our esthetic textbooks. It is a French term that relates to broken veins (telangiectasia) and diffuse redness (blotchiness).
Rosacea
Rosacea is different from a vascular lesion. Think of it as an overall description of a disease process that can include vascular lesions. When you are dealing with a client who has rosacea, it often includes multiple issues showing up within the skin. It is a progressive skin condition, and the pathology is not fully understood. It is clear that there is an immune/vascular response and repeated episodes of vasodilatation and inflammation causes a structural alteration that presents as chronic redness and telangiectasia.
What To Do?
Vascularity in the skin is always a dermal issue that is affecting the epidermis. Humans do not have veins in the structure of the epidermis. Rather, what we see with something like a broken vein is a weakness or thinning in the epidermis. Some skin is naturally thinner in structure that others, and aging also promotes this weakness. With that in mind it is important to understand the limitations that esthetic treatments have when working with structural issues. On the face, many medical treatments also are moderately effective at improving structural issues as well. Key areas that a skin care professional can treat vascular lesions include: barrier repair, cellular health, inflammation reduction, sun protection, healthy lifestyle coaching, intense pulsed lasers (IPLs) and lasers (depending on state scope). These are discussed in more detail below.
1. Improve the Barrier
A strong and healthy barrier is the goal of every esthetic treatment plan. Issues within the skin can be improved by making sure that the skin can help heal itself as well as improve cosmetic medical outcomes by having the skin’s healing process working correctly.
A treatment plan that has this goal as an outcome is going to focus on:
- Regular facials with massage (preferably on a bi-weekly basis for one full cell cycle),
- Home care that is pH balanced (not too alkaline), and
- Avoidance of emulsifiers and any other ingredients that are known to strip the barrier.
2. Make Cells Healthy
This is done by improving desquamation and microcirculation. Superficial chemical peeling with the appropriate acid for the clients’ skin type and condition is recommended. Microcirculation can be improved with devices such as microcurrent, ultrasonic spatula and galvanic current. Diet also has a role in this target.
3. Reduce Chronic Inflammation
Chronic inflammation has been linked to many internal diseases as well as increasing the signs of aging skin. From an esthetic standpoint, it is essential that any treatments, such as a chemical peel or others that induce acute inflammatory response, be managed so that it does not turn into a chronic inflammatory response. That means a conservative approach is always best until you know how your client’s skin will heal. Products designed to reduce inflammation such as colloidal oatmeal and stearyl glycyrrhetinate are an essential in a skin care professional’s back bar as well as home-care options.
4. Protect From the Sun
Long-term exposure to UV is known to thin the epidermis and promote vascular issues. Using SPF every day is essential for long-term care, but skin that has these vascular issues also needs additional protection. The use of antioxidants like vitamin C, both externally and internally, as well as lipophilic vitamins such as vitamin A, K and E will help ensure that the skin can effectively fight off free radicals that are created daily.
5. Make Healthy Lifestyle Choices
Improved diet that includes carotenoids is essential to helping improve vascular complications as well as other issues like cardiovascular health. “Eating the colors of the rainbow” is a common approach to this as well as supplementation with astaxanthin or other carotenoid supplementation.
The benefits of exercise are well documented. The focus of increasing cardiovascular health through regular aerobic exercise also helps improve microcirculation within the skin. At least 30 minutes of exercise three days a week is the minimum for improved skin health.
6. IPL and Lasers
For vascular lesions, IPLs and lasers are recommended to start to resolve these issues. The skin must be in good health to get the best benefit. The light from the device is converted to heat to target the hemoglobin within the lesion. A good outcome is a disappearance or greying of the lesion within the treatment, followed by a disappearance within a month after treatment. It usually takes multiple treatments depending on the device, and post-treatment complications can happen. Prepping the skin is an important part of this treatment, so even if you cannot operate a laser, getting the client ready will lead to a better outcome.
Client Education
These are just a few things to consider when working with redness and broken capillaries within the skin. Understanding the skin’s structure and function is an essential first step in understanding your options for treatment. It also allows you to educate your client on what can really be improved and what may not be responsive. Remember to always under promise and over deliver. There are too many “quick fixes” that leave clients disappointed and often worse than when they started.
GENERAL REFERENCES
- http://doi.org/10.3390/diseases4030024
- http://doi.org/10.3390/nu9080866
- www.ncbi.nlm.nih.gov/pubmed/24918560
(All websites accessed Nov 9, 2018)












