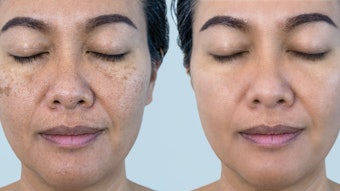
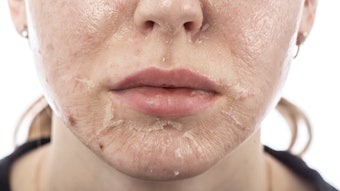
Mastering the art of extractions is one of the most important skills esthetic professionals can develop. Not only does learning how to properly extract acne lesions without creating damage in the skin set you apart in your practice, it is key to restoring the skin to optimal health.
There is, however, a fine line. Too much pressure, the incorrect tools and leaving bacteria behind can result in larger lesions, bruising, damage to cells and even scarring. How do you begin to develop this skill?
It starts with understanding the type of lesion you are working with and the client’s skin, along with a knowledge of the tools, products and techniques that support proper extraction—and which to avoid.
Types of Acne
There are many different types of acne, and understanding the root cause and how each displays in the skin will help you diagnose which type you are working with. It will be clear cut in some cases, but other times it may be a process of elimination. The primary types are explained here.
Hormonal acne (Acne vulgaris). This is the most common type of acne, primarily among adolescents. It is characterized by comedones, papules, pustules, nodules, cysts and sequelae, such as pitted or hypertrophic scars. Acne vulgaris is caused by Propionibacterium acnes (P. acnes). It typically allows for good extractions; however, the right enzymes, AHAs and other exfoliating ingredients can help do most of the work. A quality at-home system and lifestyle changes will be important to remedying this type of acne.
Cystic acne. This type is typically triggered from an excess build-up of sebum and dead skin cells. This combination blocks oxygen from reaching the cells and increases the P. acnes bacteria. Due to the tightness of the keratin in some cases, it will start to grow underneath the skin. Cystic acne can become painful and infected if you are not careful. Typically, these lesions are not extractable and forcing this can lead to scarring, which is why using ingredients that help draw bacteria to the surface is recommended. Clays, for instance, are a great partner with cystic acne. Exfoliation a few times per week and professional treatments are crucial to achieving results.
Acne cosmetica. This type of acne is caused or stimulated by cosmetics. These are usually non-inflammatory, and indicated by small and slightly raised red lesions, whiteheads and occasional pustules. This type of acne is not as common, as cosmetics have improved significantly and many products are now labeled as “non-comedogenic.” It is still important; however, to know every product your client is using to rule this out. This can usually be corrected by eliminating the acne-producing cosmetic and replacing it with a home regimen focused on cleansing and protecting.
Acne mechanica. Constant pressure, friction or repetitive physical trauma to the skin—such as rubbing from hats or other materials, phones, sunglasses, etc.—causes this type of acne. Professional enzyme treatments and a home care regimen that includes a blemish serum and all-purpose cleansing pads will help to restore skin health.
Acne rosacea. This primarily impacts adults and is more likely to occur in women than men. It is characterized by erythema with telangiectasia (small, dilated blood vessels near the surface of the skin). Lesions tend to follow the blood vessel dilation with papules and pustules forming in the center of the face, cheeks and chin. They are typically large and painful. Acne rosacea is genetic, chronic and progressive. Eliminating irritants such as excessive spicy foods, caffeine, tobacco, alcohol, saunas and stress will support the healing of this type of acne; professional peel treatments and consistent home care are also essential.
Pseudofolliculitis barbae. This is more common in men and occurs when coarse, curved hair penetrates into the skin before it leaves the follicle (also known as ingrown hairs). Salicylic acid is a key ingredient to help prevent the formation of this type acne. Mandelic acid is also a great alternative for a gentler approach. For treatment, focus on exfoliation—both physical and chemical.
Types of Acne Lesions
Along with the different types of acne, there are also varying types of lesions. These will typically fall under one of two categories: inflammatory and non-inflammatory.
Non-inflammatory acne. Non-inflammatory lesions are considered comedones and may be closed or open. Closed comedones, or whiteheads, are small, plugged follicles that are not exposed to the skin.1 Open comedones, or blackheads, occur when the follicle is dilated and the debris within becomes oxidized.2 While there is typically no infection or inflammation associated with these lesions, they can enlarge the pores and cause other issues on the surface of the skin if left untreated.
Inflammatory acne. Also referred to as cystic acne, inflammatory acne occurs when the cell wall ruptures and bacteria and sebum seep into the surrounding area to cause infection below the surface. Once the pore becomes clogged, the immune system sends white blood cells to the site to get rid of the infection. This results in inflammation.
The types of inflammatory acne includes: pustules, papules, nodules and cysts. Papules and pustules are often referred to as pimples and are the result of increased, trapped oil and bacteria inside the pore. Nodules are pockets of sebum that become hardened—they are solid to the touch and can be painful. Cystic nodules are very painful, as they occur at the deepest level. This type also has the most potential for scarring.
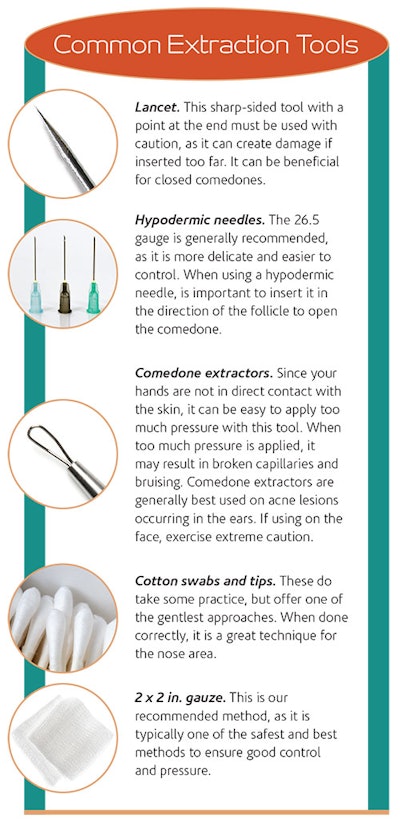
Tools and Techniques of Extractions
Acneic skin tends to have a tougher cellular wall that traps the oil and sebum, and does not allow oxygen to get in—thus creating a breeding ground for more bacteria. It is also important to understand that acne is a wound. The cells need to be healed, but the bacteria also needs to be eliminated, which is why the right tools and techniques are imperative (see Common Extraction Tools).
Extraction Protocol
Prior to turning to the aforementioned tools, prepping the skin correctly can make for much easier extractions and help prevent further or permanent damage to the skin. In other words, you can let products do the hard work for you.
Step 1: Cleanse. Cleansers with green tea and salicylic acid help reduce inflammation and remove surface bacteria and excess oil. For dry skin or those with comedones, a goat milk-based cleanser blended with natural minerals such as zeolite and essential oils support with antiseptic and antibacterial properties without stripping the skin of hydration.
Step 2: Steam. Steam may also be added during the cleansing phase to help loosen the skin and prepare it for extractions.
Step 3: Tone. After drying the skin, a toner will help remove excess lipids and continue the softening process. AHAs, BHAs and mandelic acid aid in loosening the glue-like substances (hardened keratin) around the cells, which makes it easier to extract, particularly when dealing with tighter comedones. Salicylic, L-lactic acid and green tea are ideal for someone with pustules, as these ingredients provide stronger antibacterial and anti-inflammatory support. A cell conditioner with salicylic, L-lactic acid and ursolic acid is also good to use at this point, as it will act as anti-inflammatory support and is a highly beneficial lipid reducer.
Step 4: Exfoliate (for non-inflammatory acne). When performing comedone extractions, softening the skin prior will be key. You might start with an enzyme with papaya fruit extract and papain to begin the digestion process and soften comedones for easier extraction. This may also be combined with steam, or followed with a grape seed oil hydrating serum massaged into the skin with steam to aid in cell renewal and softening. Glycolic and L-lactic acids are also good for softening, opening and loosening skin cells.
Exfoliate (for inflammatory acne). For pustule or cystic acne, AHAs or BHAs combined with hydrogen peroxide are ideal as they will help bring oxygen to the skin while stimulating the digestion process. Alternatively, a pumpkin-based enzyme with an acid strength equivalent to 10% glycolic will usher the bacteria to the surface and ready the skin for extraction. Use caution with steam, as it could over-stimulate the skin. Clay-based masks will further help draw out impurities in cystic and nodule lesions; however, if the bacteria is still reluctant to surface, peels also work well, particularly for cystic lesions.
Step 5: Oxygen Therapy. Oxygen therapy is also effective for acneic skin, since oxygen is often lacking as a result of keratin hardening below the surface, causing blockages.3 Of course, treatment will depend greatly on your client’s skin, the root cause of the acne and any other conditions present in the skin. For instance, you will want to use a lighter approach when the skin is more dry or sensitive.
Step 6: Extraction. If using the recommended 2 x 2 in. gauze, be sure that your nails are short, always wear gloves and extract everything out (especially with pustules). The goal is to reach the clear fluid after the blood—this is a sign that you have gotten everything out. Once you reach that point of blood, use a gentler pressure and rock back and forth. Fully eliminating everything is imperative. If anything is left behind, the problem can worsen.
If too much pressure is applied or an overly aggressive approach is taken on the wound, it could result in deeper damage or scarring. Start slow, focus on removing the bacteria and, when in doubt, opt for a gentler approach. The goal is to remove bacteria, reduce inflammation, heal the wounds and begin to stimulate the growth of new, healthy cells.
Step 7: Sanitize and Soothe. Immediately following any extraction, sanitation is a must. Properly sanitizing the skin will ensure that you remove any infection that may have seeped to the surface. Post-extraction support is essential. The goal is to reduce the bacteria and inflammation, and begin to soothe the skin. A toner or lotion containing green tea, L-lactic acid and salicylic acid or a mandelic acid with arginine formula (particularly for comodones) will provide antibacterial, antioxidant and cellular repair. For pustules, a green tea toner or all-purpose cleansing pads will provide gentle cleansing. Be careful to not be too aggressive with the skin post extraction, avoiding acids and high-strength enzymes.
For anti-inflammatory and healing support, a soothing balm containing Arnica montana flower extract or a vitamin E serum will reduce redness and promote healing. Ice therapy, such as chilled ice globes rolled gently over the skin, is also highly beneficial at this point for soothing support.
Step 8: Mask. You may finish with a clay and salicylic acid-based mask for healing and detoxification. Wasabi root and rosemary are also great anti-inflammatories—however, if you have performed a lot of extractions, a milk-based mask will replenish skin nutrients and provide soothing support.
Step 9: Follow up. In the initial phases, frequency is critical. Extractions may be performed once per week for up to six weeks. These can be express, 30-minute treatments if the client is coming in weekly. If done consistently, clients will begin to see inflammation significantly reduce and conditions dramatically improve.
Home Care
Home care leading up to the treatment will also aid in efficient extraction. A good pre-treatment for impacted skin might include a salicylic acid-based serum or vitamin A formula to stimulate cellular turnover. A gel with glycolic and L-lactic acid may also be used to soften comedones and reduce cellular buildup. These may be used three to four nights per week for one week leading up the treatment.
For clients in dryer climates or with more sensitive skin, a mandelic acid and arginine serum is ideal, as it will still provide rejuvenating support without being too aggressive. Again, the client’s skin will guide the best approach, and topicals and frequency should be adjusted based on oil level, dryness and when the extractions will be performed.
REFERENCES
- americanskin.org/resource/acne.php
- ncbi.nlm.nih.gov/pmc/articles/PMC1123998/
- ncbi.nlm.nih.gov/pmc/articles/PMC2585707/
(All articles accessed Dec 5, 2017.)