One of the most worrisome and prevalent skin care problems many people suffer through at some point in their lives is some degree of acne—whether it's blackheads, whiteheads, papules, pustules or blemishes. According to the American Academy of Dermatology, approximately 85% of all people have acne at some point in their lives. This common disorder can range from mild to severe, can sometimes cause extensive scarring and usually occurs between the ages of 12–50.
Development of acne
Acne is not contagious; it is caused by many different factors. Several of those factors have to exist in order for the lesions to occur. Propionibacterium acnes (P. acnes) is a bacteria that is found in every human, located inside sebaceous follicles. Those who suffer from acne have a higher amount of the bacteria than an average person. P. acnes is considered to be anaerobic, meaning that it cannot survive in the presence of oxygen. In a normal skin type, there may be P. acnes bacteria present in the follicle, but the amount remains low, because the presence of oxygen in the follicle helps to continually kill bacteria. That is one reason why exfoliation is so important for all skin types, especially for clients who are prone to breakouts—sloughing off dead skin cells will allow oxygen to reach P. acnes bacteria.
Inflammation is another factor in the development of acne. It causes a chain reaction of redness, swelling and irritation, and eventually will cause the follicle walls to become damaged. The pressure of debris—including dead cells, sebum and other biochemical factors—in the follicle will cause the walls to rupture. The debris, including the P. acnes bacteria, will move into the dermis. White blood cells arrive at the site of the rupture and release enzymes to dissolve the debris in the lesion. These enzymes affect the follicle lining, which causes more inflammation, swelling and discomfort. The enzymes even destroy collagen, potentially resulting in post-acne scarring.
Inflammatory and noninflammatory lesions
There are two types of acne lesions: inflammatory and noninflammatory. Inflammatory lesions are inflamed when blood penetrates the follicle after it has ruptured. The two prominent types of inflammatory acne lesions are papules and pustules. Noninflammatory lesions are open and closed comedones that are not red or inflamed.
A comedone consists of a mixture of dead cells and sebum that forms a plug in a sebaceous follicle and evolves from a microcomedone. There are two main types of comedones: open comedones and closed comedones, both categorized as noninflammatory acne lesions because they are not red and inflamed. Open comedones are also known as blackheads—dilated follicles in which oxygen has oxidized the sebum. Closed comedones are commonly known as a whiteheads.
Inflammatory lesions are typically known as papules and pustules. A pustule is a follicle filled with pus. Pus is a fluid comprised of millions of white blood cells mixed with follicular debris. A papule is a red bump on the skin that will typically turn into a pustule. A nodule is a very deep lesion, similar to a papule, only deeper in the dermis, and has the ability to reach the subcutaneous layer of the skin. Nodules often occur when the rupture in the follicle wall is very deep in the structure. Nodules often involve more than one follicle, which develops large pockets of infection.
A cyst is a pocketlike nodule that has a epithelial lining and a large amount of inflammation. White blood cells form a boil-like lesion that eventually ruptures. Typically, scarring is an after-effect of cystic acne. Cysts can be treated by a dermatologist who may inject the lesion with cortisone, reducing the inflammation and allowing the cyst to reduce in size. This treatment can prevent scarring.
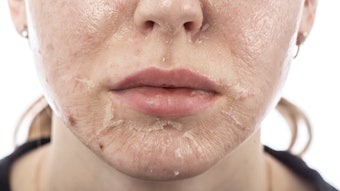
Scarring
Scars form when the skin is dealing with the inflammation and infection caused by stress-inducing lesions. Enzymes trigger white blood cells to destroy collagen while trying to recover the ruptured follicle. The enzymes, along with other immune reactions, continue to dissolve the tissue causing the scarring to occur. The immune system can also activate fibroblasts, which are collagen-producing cells, in an attempt to repair the damage from the inflammation. The collagen is produced in abundance in order to repair and replace the damaged areas. The series of events causes the collagen to clump, becoming raised and discolored. Scarring can often be improved by intralesional cortisone injections performed by an experienced dermatologist or plastic surgeon. Skin care professionals should educate their clients of all ages about the side effects of picking at lesions, also known as excoriating. This behavior can cause significant damage to the skin and rupture lesions, leading to cysts, scarring and even hyperpigmentation.
An esthetician's role
An esthetician can do nothing to change the hereditary factors that cause acne. Problem skin and acne can be brought under control to the point where there are no visible lesions for long periods of time. Clients may still have an occasional lesion, but the combination of a strict home-care regimen and a plan of action with a qualified skin care professional can greatly reduce the chances of acne returning. When you have a new client concerned with the acne lesions on her skin, one of the first questions you should ask is: “What are you currently using at home in terms of skin care and cosmetics?” Her answer will provide you with the following information:
- Why she may be experience acne;
- If she is open to investing in high-quality products based on brands she is already purchasing; and
- How educated she is regarding skin care.
Clients who have very oily skin need aggressive cleansers to remove the excess oil—foaming cleansers tend to be more aggressive. Instruct your clients to use a cleanser twice daily that removes excess oil and assists in killing acne-causing bacteria, but that is not so harsh that it will the strip the acid mantle, causing more oil production to compensate for the stripping and irritation of the stratum corneum. Recommend products to your clients that exfoliate the follicle and prevent the formation of future comedones. Medicated antibacterial agents that kill P. acnes bacteria include benzoyl peroxide gels that can vary in percentages (2.5%, 5% and 10% concentrations), and sulfur and salicylic acid in gel or liquid form. Alpha hydroxy acids (AHAs), including glycolic and lactic acids, are also excellent follicular exfoliants. For acne-prone skin, AHAs are lightweight in a gel or liquid formulation. Salicylic acid is a beta hydroxy acid and is more efficient for an acne client because it has the ability to reach inside the follicle and loosen the buildup of dead skin cells while acting as an anti-inflammatory.
Over-cleansing or over-exfoliating can strip and irritate acne-prone skin, and may result in inflammation that can lead to more flareups. In fact, there is a type of acne known as acne detergicans, which is caused from over-cleansing the skin. Once inflammatory lesions have cleared, a client may be able to reduce the strength of the treatment. Your client can continue to use stronger acne products as a spot treatment when an acne lesion is present. Explain to your clients that environment can play a significant role in the cause of acne lesions. For example, high humidity does not allow oils to evaporate easily from skin, causing sebum to stay on the skin’s surface, which results in more acne lesions.
Clear expectations
As a skin care professional, you will encounter many clients who are struggling with acne and looking to you for answers to achieve radiant skin. Supply them with clear expectations, including a structured plan that consists of a series of professional treatments and a daily at-home regimen, and they will see improvements in their skin’s clarity, and ultimately build a strong relationship with you to continue and maintain their desired results.
GENERAL REFERENCES
- www.patient.co.uk/health/acne (Accessed Oct 3, 2013)
- P Begoun, The Original Beauty Bible: Skin Care Facts for Ageless Beauty, Beginning Press, Renton, WA (2009)