Silently and efficiently, the cells of the skin work furiously to repair the damage that is incessantly assaulting your deoxyribose nucleic acid (DNA). Without these repair mechanisms, life would be impossible.
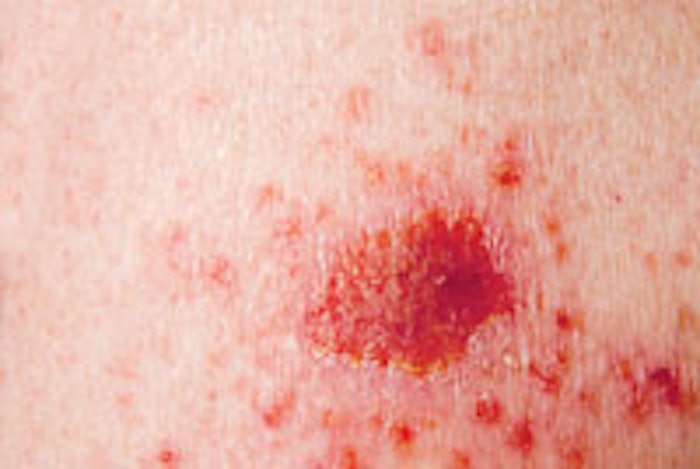
The major manifestation of DNA damage on the skin is skin cancer. Clients who have red hair and are Fitzpatrick Type I are the most susceptible to this type of damage, but anyone who is exposed to high levels of sun exposure is a candidate for DNA damage. If serious, most DNA damage to the skin will manifest as some type of lesion. If skin care professionals notice actinic keratosis, multiple ugly, pigmented spots or any lesion that cannot be recognized, they should immediately refer the client to a dermatologist.
In this article, only the basic mechanisms of DNA repair will be covered for the skin care professional by answering four essential questions.
- How does the skin become damaged?
- What type of damage is incurred by DNA and other organelles in the skin?
- How does the skin repair this damage?
- What can be used topically to assist in DNA repair?
There are so many assaults on the DNA during the life of the average cell that, eventually, if an organism lived long enough, the cells would not be able to keep up the repair effort, and they would either die or become malignant. It’s important before proceeding into this complex subject that you understand the basic structure of DNA.
What is DNA?
DNA is a very long molecule that looks much like a ladder twisted into a spiral. The two uprights of the ladder are made up of a sequence of sugar and phosphate molecules, joined end to end. The two uprights are then joined together by pairs of four bases that make up the rungs of the ladder. Chemically, these bases are known as purines and pyrimidines.
Adenine and guanine are purines bases, and thymine and cytosine are pyrimidine bases. The bases can only join in one way: adenine (A) joins to thymine (T) and guanine (G) joins to cytosine (C). Much of DNA repair has to do with restoring or replacing these bases.
How does the skin become damaged?
It has been estimated that an individual cell can suffer up to one million DNA changes per day.1 Assume that the skin contains 16% of body weight, and assume that there are 60 trillion cells in the body. Calculating the enormity of the insult would involve multiplying 9.6 trillion cells by one million hits per day per cell on the skin’s DNA! It is an extraordinary amount of damage to the body’s hereditary material. In the metabolic activities of human cells, UV light and radiation can cause DNA damage, altering or inhibiting the cell’s ability to transcribe the genes. Other potentially harmful mutations in the cell’s genome can affect the survival of its daughter cells after the cell has undergone mitosis. Following are the types of DNA damage and how the cell repairs that damage.
Skin, sunlight and cancer—molecular mechanisms. UV light is associated with two forms of skin cancer: basal cell carcinoma, (BCC) and squamous cell carcinoma (SCC). The reaction of the UV photons with cellular DNA results in absorption of these photons, which produces an excited state in the DNA. The excited molecular state results in rearrangement of the electrons, with the formation of unfavorable photo byproducts. Molecules cannot exist with this extra energy. They can get rid of it in two ways, either by irradiating it as heat or light, or by changing their molecular configuration to accommodate the extra energy. There are two known photo products produced called dimers. A dimer is two bases joined side by side in a single DNA strand, such as T-T. The two photo products are cyclobutane pyrimidine dimer (CPD) and pyrimidine-pyrimidone (6-4).
UVB radiation is the cause of the formation of abnormal molecules called adducts.2 Keep in mind that UVB is 10,000 times more mutagenic than UVA. The specific mutation induced by UVB in the DNA appears to be single-base substitutions of cytosine for thymine, a C to a T. If this substitution is not repaired, it will ultimately lead to a transcription error, in some cases producing cancer. An example of a disease produced by unrepaired DNA is xeroderma pigmentosum. This disorder is caused by a mutation in one of the 20 genes required in the repair pathway, which increases the risk of skin cancer 2,000 times. One of the paradoxes discovered in recent research is that the pyrimidine-pyrimidone (6-4) dimer is far more mutagenic than CPD, but the pyrimidine-pyrimidone (6-4) is 15 times more efficiently repaired then CPD .
Types of damage incurred by skin cells and the DNA
Cells are subjected to many types of damage, both from internal and external causes. Following are the most common types of internal DNA damage.
- Oxidation of bases from reactive
oxygen species (ROS). - Alkylation of bases, usually methylation.
- Hydrolysis of bases, such as deamination.
- “Bulky” adduct formation, in which errant molecules attach to the bases.
- Mismatch of bases due to errors in DNA replication, in which the wrong DNA base is stitched into place in a newly forming DNA strand, or a DNA base is skipped over or mistakenly inserted.
- Monoadduct damage, caused by changes in a single nitrogenous base of DNA and adduct damage.
- Damage caused by exogenous agents.
One common example of an external cause involves exposure to sunlight, which every skin care professional knows is not good in any excess form. UVB light causes cross-linking, mainly between cytosine and thymine bases, which produces pyrimidine dimers, causing direct DNA damage. UVA light creates mostly free radicals that produce indirect DNA damage. Ionizing radiation, created by cosmic rays, causes breaks in DNA strands. Thermal disruption at elevated temperatures, such as can be produced at the beach by infrared rays, increases the rate of depurination (loss of purine bases from the DNA backbone) and single-strand breaks.
Industrial chemicals, such as vinyl chloride and hydrogen peroxide, create a huge diversity of DNA adducts. Environmental chemicals, such as polycyclic aromatic hydrocarbons found in smoke, soot and tar, create adducts, including ethenobases, oxidized bases, alkylated phosphotriesters and cross-linking of DNA, to name just a few.
How the skin repairs damaged DNA
There are several ways the skin repairs DNA that has been damaged, including the following.
Direct repair of damaged bases. In a few cases, direct repair is possible, as is the case when the covalent modifications of nucleotides can be reversed by specific enzymes. For example, photolyases can repair thymine dimers induced by UV light. It splits the dimers, thereby restoring the DNA to its original condition.
Base excision repair. This involves a category of enzymes known as DNA-N-glycosylates. These enzymes can recognize a single damaged base, and cleave the bond between it and the sugar in the DNA. It then removes one base, excises several around it and replaces them with several new bases.
Nucleotide excision repair (NER). An important general process for DNA repair is NER. The process nicks DNA around damaged bases, removing a region. DNA polymerase synthesizes, and then inserts, the proper base, and the enzyme, ligase; then completes the repair. This type of system can repair many types of DNA damage, including thymine dimers and chemically modified bases. NER is found in all eukaryotes; however, the molecular mechanism is better understood in prokaryotes.
Several human diseases have been shown to involve inherited defects in genes in NER. Two of these include xeroderma pigmentosum and Cockayne syndrome. Both conditions are characterized by an increased sensitivity to sunlight. This disease is generally inherited by consanguinity, or near-relative mating, commonly called inbreeding or incest. Xeroderma pigmentosum can be caused by defects in seven different NER genes. It is the most commonly described condition attributable to a defect in the excision repair mechanism.
Mismatch repair system. DNA polymerase has an activity that recognizes mismatched bases, and is able to excise and repair them. For example, if a thymine is put in place of a cytosine across from a guanine base, the DNA polymerase recognizes this and excises the thymine, synthesizes a guanine and replaces it in the DNA. There is a backup if the proofreading system fails.
In mammalian cells, the mismatch repair system finds these errors on newly synthesized strands and corrects them. In the previous example, where a thymine has been placed across from a guanine base, a mismatch has occurred. As mentioned, thymine can only join with an adenine base. The cell must remove the thymine and replace it with a cytosine, which is the proper base to join up with a guanine base.
Repairing strand breaks. Ionizing radiation and certain chemicals can produce both single-strand breaks, affecting only one upright of the ladder; and double-strand breaks, affecting both uprights in the DNA backbone. Breaks in a single strand of the DNA molecule are repaired using the same enzyme systems that are used in base excision repair.
There are two mechanisms by which the cell attempts to repair a complete break in a DNA molecule. The first is direct joining of the broken ends. This requires proteins that recognize and bind to the exposed ends and bring them together for ligating. They would prefer to see some complementary nucleotides, but can proceed without them, so this type of joining is also called non-homologous end joining (NHEJ). A protein called Ku is essential for NHEJ. Two diseases that are characterized by strand breaks,and translocation of segments of chromosomes, are Burkitt’s lymphoma and B-cell leukemia.
Repair of mitochondria. Although mitochondrial DNA (mtDNA) was originally thought to lack DNA repair activity, four decades of research on mitochondria have revealed multiple mtDNA repair pathways, including base excision repair, single-strand break repair, mismatch repair and possibly homologous recombination. These mtDNA repair pathways are mediated by enzymes that are similar in activity to those operating in the nucleus and, in all cases identified so far in mammals, they are encoded by nuclear genes.3
What can be used topically to assist in DNA repair?
UVA and UVB cause different biological effects on the skin. UVA radiation penetrates the epidermis, resulting in damage to the dermis. Furthermore, UVA is mainly responsible for indirect DNA damage.
Meanwhile, UVB is mostly absorbed in the epidermis, and its main mechanism of action is the direct interaction with DNA via the induction of DNA damage. In the aging process, the various DNA repair systems decrease their ability as a result of the accumulation of mutagenic DNA photoproducts. Reactive carbonyl species (RCS) are potent mediators of cellular carbonyl stress originating from chemical processes. Trans-4-hydroxy-2-nonenal (4-HNE) is one of the most abundant and cytotoxic of the RCS. 4-HNE reacts with a variety of nucleophilic sites in DNA and proteins, generating various types of adducts. Intracellular RCS are suggested to play an important role in oxidative stress through their inhibitory effect on DNA repair mechanisms, as well as on induction of DNA damage through its direct interaction with repair proteins.
Preventhelia from ingredient manufacturer, Lipotec, is a tetrapeptide born from preventive cosmetics that protects skin cells from UVA-induced DNA damage and is able to promote the DNA repair system capacity, providing skin protection of intrinsic and extrinsic aging. The protective activity of Preventhelia on human epidermal keratinocytes and human dermal fibroblasts was tested in the presence of a cytotoxic dose of simulated solar light. Preventhelia increased cell viability by more than 13,000% respect to irradiated control cells.
Another ingredient, Roxisomes from Barnet Products Corporation, claims to help repair DNA damage from ROS generated by UVA in sunlight. Roxisomes contain a purified repair enzyme that recognizes the most common form of oxidative damage to DNA and helps initiate the repair process. The enzyme is delivered into the skin using a liposome technology that has been successful with other enzymes.
Of course, an ounce of prevention is worth a pound of cure, so, in order to help avoid DNA damage, advise clients to always use at least a 30 SPF sunscreen daily.
REFERENCES
- Lodish, H., et al. Molecular Biology of the Cell, 5th ed. (New York, Freeman, 2004)
- Grossman, D. Leffell, D The molecular basis of nonmelanoma skin cancer. Arch Dermatol. 1997;133;1263-1270
- Kazak L Reyes A, Holt IJ. Minimizing the damage: repair pathways keep mitochondrial DNA intact. Nat Rev Mol Cell Biol. 2012 Oct;13(10):659-71.
Michael Q. Pugliese became the third-generation CEO of Circadia by Dr. Pugliese, Inc. in 2006. Under his leadership, the Circadia brand has grown to achieve international recognition and distribution. He is a licensed esthetician, a member of the Society of Cosmetic Chemists and regularly attends its education events to stay on the cutting edge of new product development.
Peter T. Pugliese, MD has devoted himself to the study of skin physiology and influenced the course of professional skin care around the globe. Pugliese has contributed chapters to more than a dozen books and published more than 60 scientific papers. He has authored four books, including the first textbook written for estheticians by a physician, Advanced Professional Skin Care (Milady, 2005). He also is the co-author of Physiology of the Skin: Third Edition (2011). He is a member of the 2014–2015 Skin Inc. Editorial Advisory Board.










