The American Cancer Society defines cancer as “…a group of diseases characterized by uncontrolled growth and spread of abnormal cells. If the spread is not controlled, it can result in death.” According to the National Cancer Institute, of the 1,638,910 new cancer diagnoses that were predicted for 2012, 577,190 of those diagnosed were not expected to survive. Although that is 1,500 deaths per day from some type of cancer, that number is likely lower than it could be due to targeted treatment plans administered by many highly skilled physicians and other medical professionals. One common component of any cancer treatment plan is chemotherapy. Although highly effective at treating many cancers, it does have myriad negative side effects.
A side effect that is quite common, but not generally discussed, is cutaneous hyperpigmentation. Once patients have successfully completed their cancer treatments, helping them to reclaim healthy skin can be a great emotional support. By understanding the potential causes of hyperpigmentation as related to chemotherapy, you can help your patients look and feel healthy and beautiful by suppressing it during chemotherapy and addressing it after treatment is completed.
Chemotherapy: A primer
To break down this complicated topic to its basics does not do the science and effort behind drug development justice; however, because the topic of this article is hyperpigmentation and not chemotherapy, providing a basic understanding of what these drugs do in the body is useful and relevant to the skin care professional.
Because cancer cells typically replicate much more quickly and frequently than normal cells, chemotherapy drugs target the genetic material inside the nuclei of cells that are splitting, thereby stopping their replication. Some drugs inflict this damage to the chromosomes prior to the cell dividing and some while they are splitting. Using a combination of these drugs increases the number of cells that can be targeted. Cells that are not actively replicating are less likely to incur damage from the drugs; yet noncancerous, healthy cells are usually collateral damage. Hair and skin cells are constantly replicating, so they are usually damaged during these necessary treatments.
Some common cutaneous side effects of chemotherapy treatment include:
- Sensitivity or allergic reactions;
- Severe dryness;
- Flushing;
- Hyperpigmentation;
- Photosensitivity;
- Rashes; and
- Folliculitis, an acnelike skin rash.
Many of these side effects can be kept at bay with proper daily care and professional treatments. Controlling inflammation and dehydration are important for clients undergoing cancer treatment. With proper care, hyperpigmentation can also be kept under control.
Why hyperpigmentation?
After battling cancer and its effects on a person’s body and sense of self, having a skin care professional as a partner in the journey back to skin health—and to feeling beautiful—is important. Although there are many more dramatic and serious physiological side effects of chemotherapy than hyperpigmentation, helping your clients once again feel positive about their appearance is a gift. Hyperpigmentation is not a condition that is dangerous and much of the chemotherapy-induced discoloration may even fade on its own over time; however, it can be cleared much more quickly with professional treatment.
It is not entirely clear why chemotherapy causes hyperpigmentation and there seems to be a variable incidence based on the types of drugs being administered. What is known is that inflammation is a key driver in the stimulation of melanogenesis; therefore, the inflammation that commonly presents with chemotherapy likely plays a role. In general, hyperpigmentation is the deposition of melanin due to the stimulation of melanogenesis—the process by which pigment is produced and duplicated in the skin.
Prevention during the course of treatment
Extreme skin dryness, irritation and allergic reactions are all common during chemotherapy, and any of these conditions can instigate or worsen hyperpigmentation due to an increase in inflammation. Keeping the skin hydrated and calm are key steps in preventing additional hyperpigmentation.
Maintaining well-hydrated skin prior to starting a series of chemotherapy treatments is enormously important. Safe and gentle ingredients, such as urea, glycerin, hyaluronic acid, sodium pyroglutamic acid (PCA) and other humectants should be a part of these clients’ daily regimens. These types of ingredients draw moisture from the dermis up into the epidermis, plumping and hydrating the skin while improving overall skin function. It is equally important to use light occlusive agents, such as squalane, niacinamide, dimethicone and cyclomethicone, to bind and retain this increased moisture within the skin. Well-hydrated skin will be poised to handle chemotherapy with fewer complications.
Folliculitis is an inflammation or infection of the hair follicles. During chemotherapy, what is often identified as acne is actually folliculitis. It is believed that the drugs used during treatment cause follicular irritations, drawing leukocytes, or white blood cells, to the follicle. Folliculitis can appear on the face, the scalp or anywhere on the body, and needs to be addressed gently, because this compromised skin is hypersensitive and prone to reactions. Traditional acne treatments are too harsh for this condition and could result in greater reactivity, follicular distress and hyperpigmentation. Gentle products that reduce inflammation, fight bacteria and clear the follicles of cell debris—such as low percentage salicylic acid, azelaic acid, hydrocortisone, resveratrol, bisabolol and white willow bark—will help shorten the duration of the outbreak.
It is important to use gentle melanogenesis-inhibitors before, during and after treatment to suppress the instigation of melanogenesis and pigment deposition. Due to the fact that many of the common melanogenesis-inhibitors can be topically irritating, it is absolutely critical to only use ingredients that are not drying, stimulating or irritating once a client is undergoing cancer treatment. You must be especially careful with hydroquinone, because it is likely to irritate this sensitive, allergic reaction-prone skin.
Some effective melanogenesis-inhibiting ingredients include the following.
- Arbutin. Naturally found in wheat, pears, bearberries, blueberries and cranberries, arbutin suppresses the activity of tyrosinase and inhibits melanosome maturation.
- Azelaic acid. Naturally found in many grain products and castor beans, azelaic acid provides antiproliferative and cytotoxic effects on melanocytes—but not the surrounding healthy cells—and inhibits tyrosinase activity.
- Glycyrrhiza glabra root (licorice root) extract. This ingredient suppresses the tyrosinase activity of melanocytes without cytotoxicity.
- Kojic acid. Naturally found in soy, mushrooms and rice bran, kojic acid chelates copper bound to tyrosinase, and decreases the number of melanosomes and dendrites.
- L-ascorbic acid. This ingredient is naturally found in many botanical sources, such as citrus fruit and corn, and converts DOPA quinone back to L-DOPA, preventing melanin formation.
- Lactic acid. Naturally found in milk and sugars, lactic acid suppresses the formation of tyrosinase.
- Morus bombycis root (mulberry root or white mulberry tree) extract. This ingredient inhibits tyrosinase activity, particularly the conversion of tyrosinase to L-DOPA.
- Phenylethyl resorcinol. Synthetically produced, phenylethyl resorcinol inhibits the conversion of tyrosinase to L-DOPA.
- Phytic acid. Found naturally in various types of grains, bran and seeds, phytic acid inhibits the activity of tyrosinase while also inducing the exfoliation of superficial melanin-filled skin cells.
- Retinoids. Synthetically produced, retinoids suppress the activity of tyrosinase, decrease the amount of melanosomes and inhibit melanosome transfer.
- Rumex extract. Naturally found in various herbs, rumex extract inhibits the activity of tyrosinase with no irritation.
- Undecylenoyl phenylalanine. Synthetically produced, undecylenoyl phenylalanine prevents the synthesis of the melanocyte stimulating hormone (MSH) and, as a result, the formation of tyrosinase, melanin and melanosome transfer.
During the course of chemotherapy, clients should avoid the use of products containing dyes, perfumes or other known sensitizers. Additionally, good hydration, anti-inflammatory ingredients and topical steroids can bring relief to this severely stressed skin. Keeping inflammation in check regardless of the cause is helpful in controlling the incidence of hyperpigmentation.
Everyone should be using a broad-spectrum SPF of 30 or greater every day on any exposed skin. UV-induced inflammation is one of the primary causes of hyperpigmentation; therefore, SPF is an important addition for suppressing it, while also protecting the general health of the skin. Clients must understand that the SPF rating of a product only relates to its ability to protect the skin from UVB rays. Products should also offer protection from long- and short-wave UVA rays. With the new U.S. Food and Drug Administration (FDA) sunscreen monograph rules that went into effect in December 2012, only products that have undergone rigorous testing to prove their ability to protect against UVA and UVB rays can be labeled “broad-spectrum.” Protective clothing, wide-brimmed hats, sunglasses and general sun avoidance should be considered, especially between the hours of 10 am–4 pm.
Getting back to healthy, beautiful skin
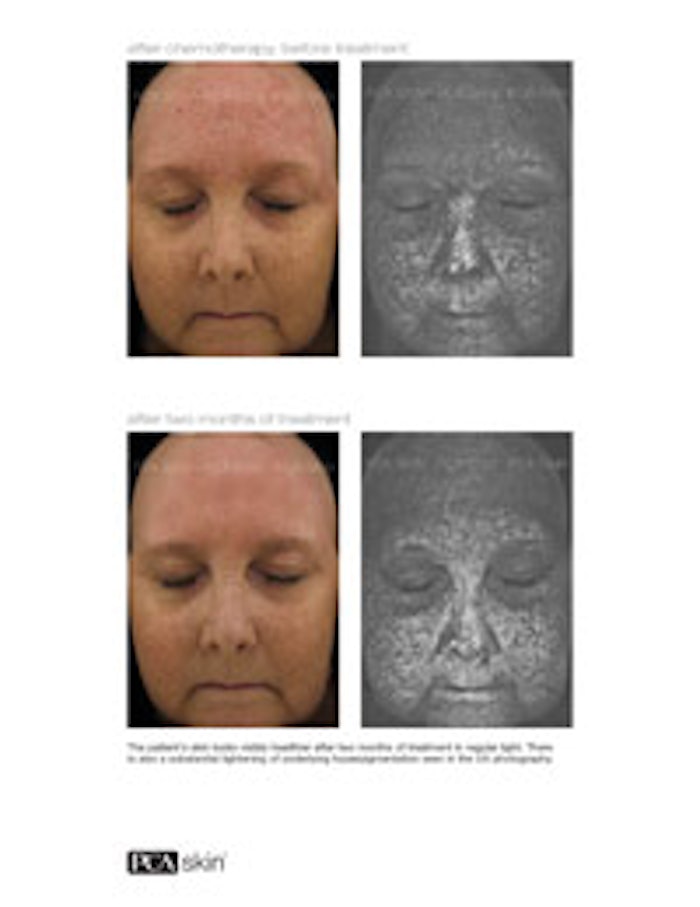
Once a client has completed chemotherapy, her skin will be ready for professional treatments rather quickly. It is best to avoid any exfoliating treatments during chemotherapy, but they are highly recommended after. If clients have followed your suggested skin care regimen during their cancer treatments, hyperpigmentation will likely not be visible on the surface; the use of an ultraviolet imaging camera, however, will typically show a marked increase in hyperpigmentation lying just below the surface. If left untreated, this discoloration will rise as the skin naturally turns over and desquamates. Some pigmentation will fade on its own, while much will deposit on the surface. Professionally applied, gently blended chemical peels every three weeks will help to improve the skin desquamation, rid the skin of its dull, impacted surface and help to speed the removal of underlying hyperpigmentation. Consider using peels formulated with multiple peeling agents at lower levels rather than a single acid peel. Straight acid peels can be aggressive and cause undue inflammation that will often worsen hyperpigmentation. There are also peeling blends available today that include melanogenesis-inhibiting ingredients to speed the clearing of unwanted pigmentation.
It is increasingly important for physicians and skin care professionals to address the common cutaneous side effects of cancer therapies with their clients and guide them to resources that can help. As the body’s largest organ, the skin of those undergoing chemotherapy has an overwhelming task. With the knowledge and tools, the skin care professional can be an important ally to the cancer patient. With proper care, hyperpigmentation can be held at bay during treatment and successfully cleared post-treatment, resulting in glowing, even and healthy skin.

San Francisco; is a spokesperson for The Skin Cancer Foundation; and is a member of the American Academy of Dermatology (AAD), the American Society for Dermatologic Surgery (ASDS) and the American College of Mohs Micrographic Surgery and Cutaneous Oncology (ACMMSCO).










