Editor’s note: This article is based on the book Health-challenged Skin: The Estheticians’ Desk Reference (2012) by Mórag Currin,. Also, a presentation based on this article by Kris Campbell of Tecniche will take place during the Advanced Education Conference Program at Face & Body® Midwest in Chicago on March 9, 2013. To register, log on to www.FaceandBody.com/midwest/register.
The professional skin care industry is often in a better position than the medical industry to deliver preventive health care recommendations, providing services in an environment that can actually help people make long-lasting lifestyle changes, which is the most effective path to disease prevention and optimal health.
In order to fulfill these needs, skin care facilities must consider adjusting their business models to encompass fitness, complementary medicine and spirituality/mental health treatments. Because people today are living longer, more are developing health issues as a result of their lifestyles. Knowledge about common diseases and syndromes makes a visit to the spa for clients with illnesses far safer and more acceptable. In Part I of this article, diabetes will be discussed, including the type of skin reactions experienced, as well as ingredients and modalities that are safe to use with this client. Not every person is going to have the same set of reactions as the next, so each client needs to be addressed based on their own personal issues resulting from their diseased state.
Diabetes
Diabetes mellitus, commonly known simply as diabetes, is a chronic health condition where the body is unable to produce enough insulin and properly break down sugar (glucose) in the blood. Glucose comes from food and is used by the cells for energy. Glucose is also made in the liver. Insulin is a hormone produced by the pancreas, and it is needed to move sugar into the cells where it can be used for energy necessary for the body’s processes.
According to Merriam-Webster, type 1 diabetes is a form of diabetes mellitus that usually develops during childhood or adolescence, and is characterized by a severe deficiency in insulin secretion resulting from atrophy of the islets of Langerhans, and causing hyperglycemia and a marked tendency toward ketoacidosis. Type 2 diabetes is a common form of diabetes mellitus that develops especially in adults and most often in obese individuals, and is characterized by hyperglycemia resulting from impaired insulin utilization coupled with the body’s inability to compensate with increased insulin production.
Throughout time, diabetic clients develop skin complications from the long-term effects of diabetes on the microcirculation and on skin collagen. Infections in the skin are more common in type 2 diabetes, while autoimmune-related lesions are more common in type 1.
Diabetic clients who have had this disease for many years have a tendency to develop complicated skin problems. Skin problems can also arise in the short-term from insulin and oral hypoglycemic drugs. One of the biggest problems with diabetes-related skin lesions is that they may serve as a port of entry for secondary infections.
Skin issues from diabetes
Several of the skin problems that can be encountered by skin care professionals working with diabetic clients include the following.
Acanthosis nigricans. This condition presents as hyperpigmented, velvety plaques in body folds. The dark color is due to the thickening of keratin-containing superficial epithelium. Although these lesions are generally asymptomatic, they can be painful, smell bad, or soften and become thinner. The most effective treatment is a change in lifestyle, which includes weight loss and exercise to reduce insulin resistance. This condition is reversible with weight loss if it is seen as a complication of obesity. If the lesions are asymptomatic, they need no treatment. Ointments containing salicylic or retinoic acid can be used to reduce thicker lesions in areas of softness/thinning in order to decrease odor and promote comfort. Systemic isotretinoin improves acanthosis nigricans, but it recurs when the drug is discontinued.
Scleredema diabeticorum. This condition is characterized by a noticeable thickening of the skin on the back of the neck and the upper back, and can extend to the shoulders and lower back area. A peau d’orange appearance of the skin can occur, often with decreased sensitivity to pain and touch.
Skin tags. These are small, stalklike, soft, often-pigmented lesions occurring on the eyelids, neck and underarm area. Treatment is not necessary, but skin tags can be removed with cryotherapy or electrodessication. They may be a sign of impaired glucose tolerance, diabetes and increased cardiovascular risk.
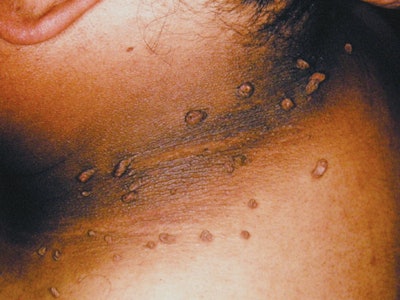
Skin-thickening. This may increase with aging diabetic clients. At first, this condition is generally asymptomatic, but there is measurable thickening that often becomes apparent in the skin on the fingers and hands. There is also a form of thickening called diabetic scleroderma, where the dermis of the upper back becomes noticeably thickened. The thickening of the skin on the hands may occur with 20–30% of all diabetic clients, regardless of the type of diabetes from which they suffer. Skin manifestations can range from pebbled knuckles to diabetic hand syndrome. Pebbled knuckles manifest through multiple minute papules found on the fingers, especially where they are stretched or straightened out on the knuckles. Stiffness is common with diabetic hand syndrome, and it can start to limit joint mobility. Skin on the hand may also present as waxy.
Vitiligo vulgaris, or hypopigmentation. This occurs more often during type 1 diabetes. These clients should be advised to avoid the sun and to use broad-spectrum sunscreens at all times, particularly in the areas hypopigmentation is occurring.
Professional responsibility
When a diabetic client considers professional skin care treatments, there will always be questions, such as: “Does the skin care professional know anything about diabetes?” and “Can she safely perform a spa treatment on a diabetic client?” One of the biggest concerns with diabetes is neuropathy, due to a lack of feeling in localized areas during electrolysis, pedicures and waxing. Clients need to be asked if they are aware of any open wounds, especially on the hands and feet. Also, it is crucial to use and recommend products with beneficial ingredients for this condition. (See Beneficial Ingredients for Diabetic Clients.)
Ask your diabetic clients if they have a continuous glucose meter (CGM) placed into their skin. These cannot be used in and around water. Also ask when insulin was last taken, because skin care treatments should not be performed during the peak of insulin activity. Intermediate-acting insulin taken in the early morning allows for a safe spa treatment mid-afternoon, whereas rapid-acting insulin allows for a safe spa treatment approximately one-to-three hours after administration.
There are many other skin manifestations to take into consideration if the skin care professional is working with the appendages of diabetic clients. (See Additional Skin Manifestations.) Dealing with pedicures requires more knowledge about diabetes and risks. Training is available for nail technicians to deal with diabetes through a variety of organizations, such as the International Pedicure Association. There is more and more awareness about diabetes in the professional skin care industry, and more training opportunities are becoming available on the topic.
Some studies have suggested that regular massage may help normalize blood glucose in diabetic clients, as well as reduce anxiety, headaches, depression, work stress and anger. However, further studies are needed to clarify the benefits that massage may have as a complementary treatment for diabetes. Although there is no evidence that massage itself is harmful or contraindicated for people with diabetes, some aspects of the condition mean that massage for diabetics should be chosen carefully to prevent any adverse effects.
Professional skin care treatments must be dictated by the client’s current condition at the time of treatment. The client may require many adjustments to any treatment provided. Only by working hand-in-hand with clients will the right course of treatment be determined.
In Part II of this article, which will appear in the March 2013 issue of Skin Inc. magazine, the skin issues related to clients with celiac disease and systemic lupus erythematosus will be detailed, along with ingredient and treatment suggestions when working with these types of clients.
Mórag Currin is an esthetic instructor with more than 19 years of spa industry experience, and more than 10 years of training and training management experience. She pioneered the Oncology Esthetics advanced training for spa professionals, and is the author of Oncology Esthetics: A Practitioner’s Guide (2009) and Health-challenged Skin: The Estheticians’ Desk Reference (2012).