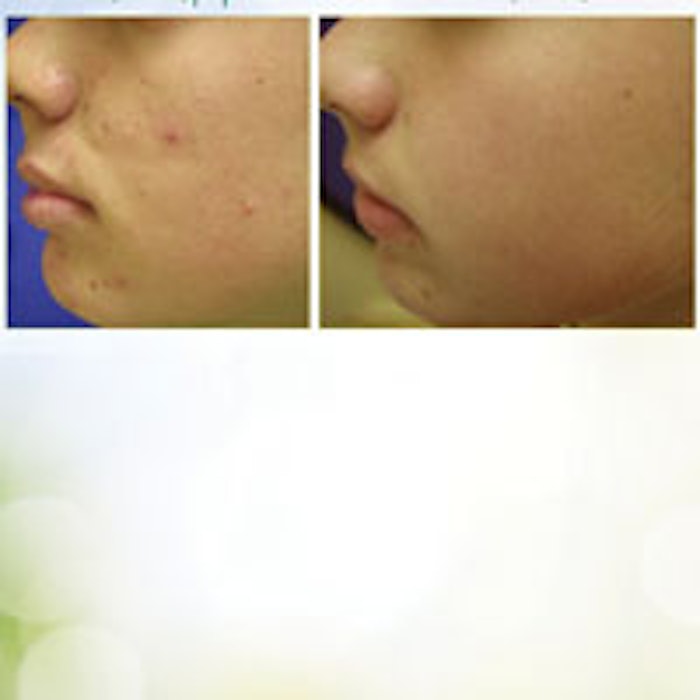
Acne is a common skin disorder affecting both genders and all ethnic groups. In fact, the condition affects at least 80% of adolescents and young adults to some degree. Research also shows that a large number of women over 25 have acne, and the prevalence of acne remains constant until approximately 44, at which time there is a decrease in its incidence.1 It is important to understand the epidemiology and causes of acne and oily skin to truly appreciate the science and benefit behind today’s acne treatment products.
Acne can substantially impact a client’s quality of life. Clients with moderate or severe acne generally have higher levels of behavioral and emotional difficulties than those with clearer skin. The most prominent psychological impact acne has on clients is lower self-confidence, embarrassment, and reduced self-esteem and self-image. The psychosocial impact of this skin condition should never be underestimated.
Clinical features and etiology
Acne is a self-limiting disease that involves the hair follicle (pilosebaceous) unit. A pilosebaceous unit is comprised of a follicle or pore and an oil gland (sebaceous gland). Characteristic skin lesions are created by pathology in the pilosebaceous unit and include blackheads (comedones), red papules, pustules, red nodules and cysts.
The cause of acne is multifactorial. The female and male hormones that impact the pilosebaceous gland are in higher concentrations after puberty. Stress can also influence hormone levels, related in part to increased adrenal gland secretion, causing and aggravating acne. Altered keratinization and abnormal skin cell growth in the pore create a dead skin cell/protein/lipid complex that plugs the pilosebaceous gland (microcomedone). Abnormal sebum production and swollen sebaceous glands are present in acne-prone individuals. Also, the composition of free fatty acids secreted by acne-prone individuals differs from those in acne-free individuals. Abnormal bacterial colonization in the pilosebaceous unit occurs in acne-prone individuals. Lastly, an exaggerated immune and inflammatory response to microcomedones, sebum and follicular bacteria produce papules, pustules, nodules and cysts in acne-prone individuals.
The initial lesion in acne caused by a combination of etiologies is the comedone. A comedone starts in the upper portion of the pilosebaceous gland as an expanding mass of cellular debris, keratin protein and lipid material. Bacteria (Proprionebacterium acnes) populate the blocked pilosebaceous gland. Bacteria produce an inflammatory response by the chemical breakdown of lipids within the plugged pilosebaceous unit. This starts the development of small, red papules. As they grow in size, the follicle wall thins, and the follicle itself stretches and swells. Comedones become inflamed when the follicle wall is ruptured, which releases small amounts of cellular and lipid material into the dermis—papules and pustules. Release of all the bacteria, cellular and lipid material in a single comedone produces a full inflammatory response—nodules and cysts. (Editor’s note: To learn more about the physiology of the skin as it relates to acne, check out Skin Inc. Video Education at learn.SkinInc.com.)
Rationale and ingredients
Acne is recognized as a multifactorial disease requiring a multifaceted approach to therapy. Establishing an accurate assessment is essential for developing a treatment strategy for acne and evaluating treatment success. Treatment of acne is directed at reversing the pathologic process. The mechanism of action of each treatment, and its ability to address one or more of the causes of acne needs to be evaluated when creating an acne treatment program.
Therefore, treatment must contain products that:
- Prevent abnormal epidermal cell growth;
- Normalize and enhance skin exfoliation at the opening of the pore;
- Kill the bacteria in the pore;
- Reduce the exaggerated inflammatory response; and
- Control abnormal and excessive sebum production.
Treatment is designed to heal active lesions and prevent their formation. True scarring must be distinguished from erythematous or hyperpigmented spots that can result from inflammatory acne. The latter generally resolve throughout a few months without visible marks. Acne should be treated aggressively to prevent permanent scarring.
Most acne treatment programs contain a single active ingredient, such as benzoyl peroxide. Results of clinical trials indicate treatment programs that contain multiple active ingredients working together may produce better results.2 It is important to remember that many acne clients have additional skin problems, especially women 30–50 years old. Rough skin texture, brown skin discoloration, skin dryness and fine lines can complicate the treatment of acne. A customized, multifaceted treatment regimen is needed to treat individual clients. Initially, determine the client’s skin type—sensitive vs. normal or dry-normal vs. normal-oily. This will guide the selection of a cleanser; acne solution gel, cream or lotion topical treatment; and spot treatment.
Following are some common acne-fighting ingredients.
Salicylic acid. Salicylic acid is an organic beta hydroxy acid that is a natural plant-derived ingredient. It causes cells of the stratum corneum to shed more rapidly to prevent pores from clogging and allow space for new cell growth, helping reduce and prevent blackheads. Salicylic acid is found in acne cleansers and topical acne treatments, and is designed to cleanse, exfoliate and prepare the skin to make other anti-acne ingredients more effective. Although it reduces bacteria and excess oil from the skin, its main role is correcting abnormal keratinization.
Benzoyl peroxide. The benefit of benzoyl peroxide in the treatment of acne is its ability to kill the bacteria that cause acne and oxidize the oils on the surface of the skin produced by the sebaceous glands. Benzoyl peroxide increases the pH of the skin, causing some clients to develop redness, itching, stinging and sometimes swelling of the skin. Its strong oxidative properties can bleach hair and clothing, as well as create sun sensitivity in some clients.
Glycolic acid and alpha lipoic acid. Combining these two ingredients can help correct the abnormal keratinization and the abnormal sebum secretion in acne-prone individuals. The major corrective effects are a reduction in abnormal sebum secretion and the elimination of abnormal keratinization.
Azelaic acid. This is a natural plant-derived dicarboxylic acid, and is a prescription product used in the treatment of acne. In lower concentrations, it can be obtained without a prescription, and when combined with other anti-acne products, it can help eliminate acne and hyperpigmentation. It has antibacterial and keratolytic effects on the stratum corneum. The keratolytic effect reduces the formation of blackheads and increases the penetration of the azelaic acid into the pilosebaceous gland. This enhances the antibacterial effect of the azelaic acid and decreases the P. acnes that cause inflammatory acne lesions.
Vitamin A. Retinoic acid, retinol and other retinoids are vitamin A-derived ingredients that have significant keratolytic effects on the stratum corneum. Retinoic acid, adapalene and other retinoids are only available with a prescription; however, retinol is available without a prescription.
Sulfur. Micronized, elemental sulfur—or sodium sulfacetamide—has antibacterial properties that are responsible for its ability to eliminate active acne lesions. A worry for some is that an allergy to sulfa drugs may cause them to have problems with products that contain natural, elemental sulfur; however, no one is allergic to natural, elemental sulfur. The sulfur atom is not an allergenic agent. However, sulfa drugs are more appropriately labeled sulfonamides. Sulfonamides are not allergenic, but they have the ability to form sulfonamide-protein complexes that can be allergenic in some individuals.
Allantoin. Allantoin is a diureide of glyoxylic acid and is a natural botanical extract of the comfrey plant. Its keratolytic effect enhances the desquamation of dead skin cells, and it forms complexes with irritating sebum and sensitizing bacteria that cause excess oil production and acne lesions. Controlling skin surface oil and reducing skin bacteria promotes skin healing. Allantoin reduces abnormal keratinization and reduces bacterial colonization in the pilosebaceous unit, but its major corrective effect is eliminating abnormal sebum production.
Treatment
Client expectations are a critical step in initiating therapy for acne. Realistic expectations and time lines for improvement will encourage client compliance. Typically, mild acne will improve 30–50% in 12 weeks and 60% or better by 26 weeks with appropriate treatment.3 Moderate acne or acne rosacea will improve 20–40% in 12 weeks and 50% or better by 26 weeks.3 The treatment of acne vulgaris is a long-term process that must be individualized for each client. The two most important factors for the initial treatment of acne are based on skin type, and the severity of the acne. In addition, benzoyl peroxides can oxidize other acne medications, rendering them ineffective.3 Studies indicate that there is a synergistic effect in improving acne when benzoyl peroxides are combined with other compatible anti-acne ingredients, but these are only available by prescription.3 These studies indicate that using several active ingredients that are compatible and work together to address the various causes of acne produce better and faster results than a treatment program with a single active ingredient.3 Effective cleansers can contain ingredients such as salicylic acid and glycolic acid; effective acne treatment products can contain azelaic acid, benozyl peroxide or salicylic acid; and effective acne spot treatments can contain precipitated sulfur, benzoyl peroxide or salicylic acid.
Acne treatment requires the ability to make treatment modifications for each client based on the individual acne lesions and skin type. In clients with oily skin, reducing skin oiliness increases the effectiveness of other acne medications. Clients with significant comedones will benefit from keratolytic ingredients and certain skin peels. Acne clients are not immune to sun damage and should use a hypoallergenic, noncomedogenic sunscreen on a daily basis.
Acne is recognized as a multifactorial disease that requires clinical finesse and a multifaceted approach to therapy, and the treatment of acne requires the use of scientifically advanced skin care products, as well as clinical experience.
REFERENCES
1. S Bellew, et al, Pathogenesis of Acne Vulgarus, J Drugs Dermatol 10 582–590 (Jun 2011)
2. D Thiboutot, et al, A 3-step acne system containing solubilized benzoyl peroxide versus clindamycin-benzoyl peroxide, Cutis 84(1) 48–55 (Jul 2009)
3. L Eichenfield, et al, Safety and Efficacy of Clindamycin Phosphate 1.2%-Benzoyl Peroxide 3% Fixed-dose Combination Gel for the Treatment of Acne Vulgaris, J Drugs Dermatol 10(12) 1382–1396 (Dec 2011)
Lawrence Samuels, MD, is the chief of dermatology at St. Luke’s Hospital in St. Louis, and is the founder of the skin care product line Rx Systems PF. He is an accredited dermatologist who has been transforming the lives of patients through his passion and skill for more than 30 years. Samuels is also a fellow of the American Academy of Dermatology, along with a variety of other professional organizations. His work has also been published in medical journals and texts.










