The buzz on medical spas has died down a bit, likely due to the numerous consumer articles citing safety concerns and medical supervision issues. And although there are some who say the medical spa boom is still growing, a segment of the industry that is definitely expanding is state regulatory boards’ governance.
In early 2005, the National Coalition of Estheticians, Manufacturers/Distributors & Associations (NCEA) released this definition of a medical spa: “A medical spa is a facility that, during all hours of business, shall operate under the on-site supervision of licensed health care professionals operating within their scope of practice with staff members who operate within their scope of practice as defined by their individual licensing board if licensure is required. The facility may offer traditional, complementary and alternative health practices and treatments in a spa-like setting.” The International Medical Spa Association later adopted this definition as well, and several state regulatory boards have looked to it to develop statements for their own medical spa governance.
A new legal frontier
As with any new technologies, procedures and partnerships, the slow-moving legislative climate across the country has spurred
| Web Resources |
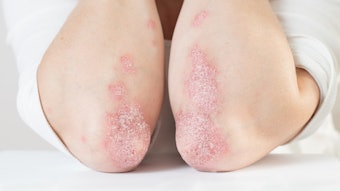
Potential negative treatment outcomes such as prolonged erythema, pigmentation problems, infection and scarring can occur in any setting. In unsupervised medical spas, these post-procedure complications can lead to serious legal problems. David J. Goldberg, MD, JD, in a recent interview states, “Redness and hyperpigmentation issues usually resolve themselves over time, and so they never usually turn into successful lawsuits against the physician or physician extender.” He goes on to say that, from a legal standpoint, the most potentially permanent problems are related to infection, scarring and pigmentation loss.
To continue reading about these issues involved with working in a medical spa, go to www.SkinInc.com.
Physician extenders
Legal issues involving the use of physician extenders—medically trained staff, typically advanced nurse practitioners and physicians’ assistants—are becoming more common because physicians are increasingly relying upon them. A 2002 American Academy of Dermatology practice profile survey showed one-third of dermatologists also use physician extenders. Are these physicians employing estheticians? Nurses? Physician assistants? The study did not elucidate on who the “physicians extenders” specifically are. However, the Society of Dermatology SkinCare Specialists has more than 300 members, of which 90% work with a dermatologist in a clinical or medical spa setting. And the Society of Plastic Surgical Skin Care Specialists has more than 500 members, all of whom work with plastic surgeons.
Legally, the physician extenders work for the physicians, who have the ultimate responsibility of whether they are physically on-site or not. According to the NCEA, a medical spa staff’s legal responsibility is toward the safety and proper care of the client. Despite the fact that there is, in most a cases, the possibility of risk or harm, such as a formerly unknown allergic reaction flaring up, a standard of care is expected and required in a medical spa setting. Your best legal strategy when working in this type of facility is maintaining a high standard of care and putting your best efforts into preventing adverse reactions and accidents—all while being mindful of your scope of practice, of course.
Legal liability
Furthermore, according to the NCEA, negligence in most legal systems is the failure to meet the duty of care expected. In the event of an accident or adverse reaction, a client may bring legal action against the practitioner and medical spa. The plaintiff, who is the client or the person suing, can claim the facility failed to meet the expectations of care, was negligent, and that it was this negligence that led to the accident, causing injury. If the practitioner and the medical spa are found by the courts to have been negligent, they will be held liable for any damages that have been determined.
The best advice is to continually check your state regulatory board’s Web site in order to stay abreast of the legislative issues you and your practice may be facing. A new rule or regulation is generally not announced to licensees—it is up to you to keep yourself and your spa staff informed. To stay consistently accurate, find out how often your regulatory board meets, and then make it a habit to check its Web site for the minutes and announcements that could potentially affect your medical spa’s operation and ultimate survival on a regular basis.
For more on ways to obtain information on state regulations, go to www.SkinInc.com.
What about the business?
Are medical spa facilities really a marriage of science and beauty? What roles do business planning and research play in them? If legal and liability issues are a major concern and statistics support the lack of orientation and training, client assessment, staffing, availability of information and leadership, then why even get into the medical spa business?
According to the U.S. Small Business Administration, more than 50% of small businesses fail in the first year and 95% within the first five years. Whether you are starting a medical spa, are looking to raise additional capital to expand your spa, or are looking to evaluate and value your facility to sell, current statistics prove you will do much better with a business plan than without. Reasons for business failure vary, but the vast majority of them can be grouped under the category of poor planning.
As you contemplate your treatment menu and choose the colors for your office’s décor, don’t forget the business plan aspect of your facility. This definitely should encompass crossing your t’s and dotting your i’s from a legal and liability standpoint as well. Ignorance of the law is no defense.