Editor’s note: This article is based on the book Health-challenged Skin: The Estheticians’ Desk Reference (2012) by Mórag Currin.
Author’s note: The author would like to acknowledge Kris Campbell and Jennifer Brodeur for their contributions to this article.
In Part I of this article, which appeared in the February 2013 issue of Skin Inc. magazine, skin challenged with diabetes was addressed, including the type of skin reactions that this client experiences, as well as ingredients and modalities that are safe to use with this client type. Following is in-depth information about issues and information skin care professionals should be aware of when working with clients who suffer from celiac disease and systemic lupus erythematosus (SLE).
Celiac disease
Celiac disease is an inherited, immune-mediated intolerance to dietary gluten. “Gluten” is the collective term for the amino acid sequences found in wheat, barley, rye and, to a lesser extent, oats, which trigger an immune reaction. When gluten is ingested, susceptible individuals mount a specific, intense inflammatory response within the small intestinal mucosa that damages the lining, and interferes with digestion and absorption.
Nutrient deficits are responsible for most symptoms in celiac disease; many are seemingly unrelated conditions. A partial list includes depression, lack of concentration, anxiety, insomnia, hypertension, obesity, alopecia, defective fingernails, edema, eczema, seborrhea, muscle abnormalities, tremors, brain atrophy, dementia, headache, chronic fatigue and peripheral neuropathy. Nutritional deficiencies inevitably affect the integrity of the skin, especially in those clients who are not aware they have celiac disease.
Because most skin care professionals provide facials, the mouth is an area of concern. Lowered saliva pH, resulting in more acidic saliva associated with celiac disease, predisposes a client to dental cavities and poor starch digestion. Be aware of other skin-related symptoms of celiac disease when working with clients who have this disease. They include the following.
Acne. Celiac disease and malabsorption, as well as hormonal upset, can contribute to a greater production of acne. Many acne-sufferers have reported relief from their skin condition when they went gluten-free. Clients may want to have their physician check to confirm their acnelike condition is not actually dermatitis herpetiformis. Because each client has different issues and possible causes of acne, different acne regimens can be tried to see which is the most beneficial for each client.
Dry skin. Also correlated to malabsorption, dry skin is a very common complaint among those with celiac disease. Dry skin, in some cases, can be reduced by a gluten-free diet, and it is recommended that these clients use emollient, gluten-free products.
Eczema. When clients have eczema, they develop patches of red, cracked skin that sometimes weep clear fluid. People with eczema seem to have both lower levels of a type of cytokine protein that’s associated with a healthy immune system and higher levels of a cytokine protein that’s involved in allergic reactions. Some physicians consider eczema an autoimmune condition. Researchers have compared the prevalence of eczema in people who also suffer from celiac disease to eczema prevalence in control subjects, and they’ve found that eczema occurs about three times more frequently in those with celiac disease and about two times more frequently in their relatives, potentially indicating a genetic link between the two conditions.
A gluten-free diet can make a difference to eczema in a celiac client, as can the use of gluten-free skin care products. Gliadin is the toxic protein fragment that causes eczema in celiac disease, so whether in the diet or through the use of topical skin care products, gliadin should not be present.
Urticaria (hives). Urticaria is an eruption of erythematous or edematous swellings of the dermis or subcutaneous tissue, and is due to a local increase of the permeability of capillaries on celiac clients. Urticaria is generally treated with oral medications; however, clients may look for alternative topical options, including antipruritic medications, such as topical steroids, including hydrocortisone. Topical antihistamines, such as diphenhydramine, works by blocking the effects of histamines. A natural product alternative includes calamine, which effectively helps soothe itching on the skin, and topical anesthetics, such as benzocaine, can relieve itchiness by anaesthetizing itch nerves. Also, counterirritants, such as mint oil, menthol and camphor, represent a more natural choice of active ingredients for anti-itch creams. A counterirritant operates by creating a diversion, producing sensations that attract your attention. Theoretically, by creating inflammation in one location, you will reduce the inflammation of another by creating antagonism between itch-processing neurons.
There seems to be some controversy about celiac disease and the use of skin care products and cosmetics that contain gluten. It makes sense that if your client has celiac disease, gluten-free products should be used.
Ingredients and treatments. Oenothera biennis (evening primrose) oil, which contains gamma linolenic acid, an essential fatty acid, has been used to ease bruises and speed wound-healing in those with celiac disease. Also, Simmondsia chinensis (jojoba) seed oil contains vital nutrients such as vitamins—especially vitamin E—and minerals, and has antimicrobial properties to assist with the healing of sores and wounds. As the oil closest to human sebum, it’s beneficial for oily, dry, red, inflamed and mature skin, as well as skin conditions such as eczema and rosacea.
According to the Canadian Celiac Association, it is important for clients with celiac disease to use gluten-free cosmetics as a precaution to ensure they do not mistakenly digest any cosmetics that could cause damage. Treating any type of health-challenged skin at a professional skin care facility takes thorough thought and ingredient consideration. Although caution is advised, most professional skin care treatments have no direct impact on the health of intestinal villi. Consequently, professional skin care treatments can neither improve nor exacerbate celiac disease.
When working with celiac clients, consider offering gluten-free facials, which should include “clean” formulas with nonirritating ingredients. While this may seem over the top, gluten-intolerant clients really need to be assured that there is no cross-contamination between bowls, implements and sheets. Skin care professionals must have integrity and not use products other than those selected for use on a client with celiac disease. If the ingredients are too active, chances are a breakout will occur. It’s important to use the least amount of fragrances, dyes and gluten possible. Throughout a certain period of time, clients will develop a gluten intolerance even when gluten is applied to the skin or scalp.
Systemic lupus erythematosus (SLE)
Lupus is an autoimmune disease where the client’s immune system creates antibodies that, instead of protecting the body from bacteria and viruses, attack the person’s own body tissues. Symptoms include extreme fatigue, joint pain, muscle aches and anemia. SLE is a disease with many manifestations, and each client’s profile is different. Lupus can mimic other diseases, such as multiple sclerosis and rheumatoid arthritis, making it difficult to diagnose.
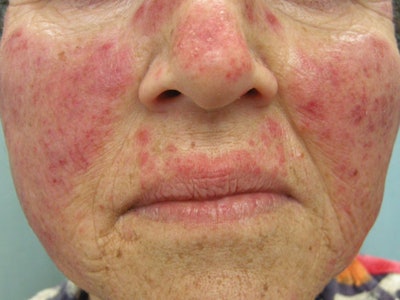
Skin problems are very common in people with lupus. Some skin rashes and lesions are very specific to lupus. Sensitivity to UV rays and some types of artificial light are responsible for aggravating these rashes or lesions. Broad-spectrum sunscreen use is strongly recommended, especially a physical block with zinc oxide. Do not use skin care products on these clients that will aggravate their skin and make it worse. Be aware of other skin-related symptoms of SLE when working with clients who have this disease. They include the following.
Butterfly rash. This rash appears over the nose and cheeks, and can range from a faint blush to a rash that is very severe, with scaling. It is very sensitive to light and appears to gets worse when skin is exposed to the sun or certain types of artificial light. The rash may be permanent, or may come and go. Some physicians treat it with steroids; however, many do not do well with this in the long term. Some clients may be on topical anti-inflammatory immunosuppressant creams, such as pimecrolimus or tacrolimus for this rash. Sunscreen is necessary on this area, and a physical sunscreen with zinc oxide should be soothing.
Discoid lesions. These scarring, coin-shaped lesions are seen on areas of the skin that have been exposed to UV light. They may also occur on the scalp and produce a scarring, localized baldness that is permanent. Sunscreen is necessary for these areas of the skin.
Drug-induced skin changes. Some drugs prescribed for lupus conditions, such as corticosteroids, immunosuppressives and antineoplastics, can also affect the skin, so consulting with the client about any side effects is absolutely necessary. Sunscreen is necessary to avoid further aggravation.
Mucous membrane lesions. Mouth ulcers are sometimes seen in SLE clients, and nose and vaginal ulcers may also occur. These lesions are usually painless. It is important to differentiate lupus ulcers from herpes lesions or cold sores, which may be brought on by the use of immunosuppressive drugs.
Subacute cutaneous lesions. These nonscarring, red, coin-shaped lesions are very sensitive to UV light; can appear scaly and can mimic the lesions seen in psoriasis; and may occur only on the face or cover large areas of the body. Sunscreen is necessary to avoid further aggravation.
Raynaud’s phenomenon. This condition occurs when the blood vessels of the fingers and toes react in an extreme way to cold or stress. They suddenly get very narrow, and the blood supply to these areas is diminished. As a result, the fingers and toes become cold, and can become pale or bluish. Pain or tingling can occur when the hands and feet warm up and circulation returns to normal. Ensure your client’s hands and feet are kept warm at all times, and avoid any cold treatments.
Vasculitis. This occurs when blood vessels become inflamed. Very small blood vessels can break and cause bleeding into the tissues, resulting in tiny, reddish-purple spots on the skin, known as petechiae. Larger spots are called purpura and may look like a bruise. Vasculitis can also cause blood clots to form, skin ulcers to develop, and small black areas to appear around fingers and toenails. If you see this condition on clients, recommend that they see their physician right away.
The most common treatments for skin lesions exacerbated by lupus are steroid creams or gels. In some cases, liquid steroids will be injected directly into the lesions.
Topical steroids are effective anti-inflammatory preparations and are available in combination with salicylic acid to enhance penetration, and with antibacterial and antifungal agents. Local side effects from topical steroids include: skin thinning (atrophy) and stretch marks (striae); easy bruising and tearing of skin; perioral dermatitis (rash around the mouth); enlarged blood vessels (telangiecstasia); and susceptibility to skin infections. Obviously, the risk of side effects depends on the strength of the steroid creams or gels, the length of application, the site treated and the actual skin condition being treated.
Topical immune-modulators have been developed to treat serious skin conditions without the side effects presented by topical steroid creams and gels. Tacrolimus ointment and pimecrolimus cream have been shown to suppress the activity of the immune system in the skin, including the butterfly rash, subactute cutaneous lupus and possibly even discoid lupus lesions.
Very often a client with severe skin issues will not seek facial treatments. Other clients will try facial treatments and explore what products may help with their skin lesions.
Ingredients and treatments
Skin care products with anti-inflammatory, soothing, protective ingredients are best for clients with SLE. Moisturizers can also be helpful for dry skin, and any lupus-related scars can be covered with a thick concealer.
Artemisia vulgaris (mugwort) extract/algae extract is a combo extract rich in amino acids, polypeptides and cellular carbohydrates. It also combats irritation and redness caused by UV exposure, chemical aggravations and the environment. This ingredient works well on erythema.
Calamine powder is anti-pruritic (anti-itch), and acts as an astringent for blisters. Calamine works well on hives and itching.
Ergothioneine (L) is a chirally correct exogenous antioxidant that protects the skin from oxidative and DNA damage, as well as protects the mitochondrial membrane against oxidation. It also transfers fatty acids into the mitochondria to help use oxygen efficiently and to produce more energy, giving the skin vitality. This ingredient works well for photosensitivity.
Professional skin care treatments are dictated by the client’s current condition at the time of treatment. If pain and inflammation is present, the client should not have a treatment or the skin care professional would have to make lots of adjustments to any treatment provided.
Enhance clients' well-being
Traditional skin care professionals who have an interest in the well-being of their clients, and who are willing to create a new spa model that encompasses health and wellness, are professionals with a successful future. Skin care professionals who are providing additional modalities with their traditional treatments will be in more demand. These are dedicated and outstanding skin care professionals, and more and more of them are rising up to the challenge. Today, with spa clients living longer, there is a need to care for the body—inside and out—and the key to joyful living and success can be obtained from knowledgeable skin care professionals.
GENERAL REFERENCES
C Ciacci, et al., Allergy prevalence in adult celiac disease, J of Allergy and Clinical Immunology 113 6 1199–1203 (Jun 2004)
BT Cooper, et al., Coeliac disease and immunological disorders Br Med J 1 537–539 (Mar 1978)
E Varjonen, et al., Antigliadin IgE—indicator of wheat allergy in atopic dermatitis Allergy 55 4 386–391 (Apr 2000)
www.niams.nih.gov (Accessed Jan 17, 2013)
Mórag Currin is an esthetic instructor with more than 19 years of spa industry experience, and more than 10 years of training and training management experience. She pioneered the Oncology Esthetics advanced training for spa professionals, and is the author of Oncology Esthetics: A Practitioner’s Guide (2009) and Health-challenged Skin: The Estheticians’ Desk Reference (2012).